Abstract
Objective:
We sought to compare two approaches to antenatal testing for their impact on the workforce.
Study Design:
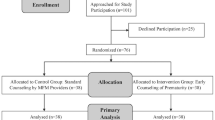
This is a prospective observational study of women who presented for antenatal testing. All women were given a survey upon presentation. As per hospital protocol, nonstress testing (NST) was performed semiweekly and biophysical profile (BPP) was performed weekly. The choice of testing was determined by the attending physician. χ2- and Student's t-tests were performed where appropriate. A P-value of <0.05 was considered significant.
Result:
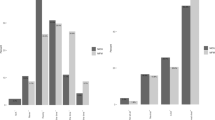
A total of 195 women were surveyed. Among them, 94 women had an NST and 101 had a BPP. Overall, 59.2% were multiparous, 33.1% had to arrange for child care and 97.2% felt reassured by the testing. There were no differences in demographic characteristics, education, type of insurance or employment status between the groups. Women who had NSTs were more likely to lose time from work than those who had BPPs (218.4 versus 68.9 min; P<0.001). Of the women who had semiweekly NSTs, 80.6% would have preferred weekly testing. If the 94 women who received semiweekly testing had weekly testing, a total of 534.4 h would have been available for the workforce.
Conclusion:
Twice-weekly NST results in a significant increase in time lost from the workforce compared with weekly BPP.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Armour S . Pregnant workers report growing discrimination. USA Today, 2/16/05 www.usatoday.com/money/workplace/2005-02-16.htm.
McCartney PR, Schmidt JV . Intrapartum fetal monitoring: a historical perspective. Fetal Heart Monitoring Principles and Practice, 3rd edn. 2003; 3–22.
American College of Obstetrics and Gynecology. ACOG practice bulletin: antepartum fetal surveillance, no. 9, 1999; Compendium 2007; II: pp 503–513.
Devoe LD, Jones CR . Nonstress test: evidence-based use in high-risk pregnancy. Clin Obstet Gynecol 2002; 45 (4): 986–992.
Lee CY, DiLoreto PC, O’Lane JM . A study of fetal heart rate acceleration patterns. Obstet Gynecol 1975; 45: 142–146.
Powell OH, Melville A, MacKenna JL . Fetal heart rate acceleration in labor: excellent prognostic indicator. Am J Obstet Gynecol 1979; 134: 36.
Baser I, Johnson TR, Paine LL . Coupling of fetal movement and fetal heart rate accelerations as an indicator of fetal health. Obstet Gynecol 1992; 80: 1.
Rochard F, Schifrin BS, Goupil F, Legrand H, Blottiere J, Sureau C . Nonstressed fetal heart rate monitoring in the antepartum period. Am J Obstet Gynecol 1976; 126 (6): 699–706.
Murata Y, Martin CB, Ikenoue T, Hashimoto T, Taira S, Sagawa T et al. Fetal heart rate accelerations and late decelerations during the course of intrauterine death in chronically catheterized rhesus monkeys. Am J Obstet Gynecol 1982; 144: 218.
Dawes GS, Fox HE, Leduc BM, Liggins GC, Richards RT . Respiratory movements and paradoxical sleep in foetal lambs. J Physiol 1970; 210: 77.
Boddy K, Dawes GS, Fisher R, Pinter S, Robinson JS . Foetal respiratory movements, electrocortical and cardiovascular responses to hypoxemia and hypercapnia in sheep. J Physiol 1974; 243: 599–618.
Devoe LD, Abduljabbar H, Carmichael L, Probert C, Patrick J . The effects of maternal hyperoxia on fetal breathing movements in third-trimester pregnancies. Am J Obstet Gynecol 1984; 148: 790.
Natale R, Clewlow F, Dawes GS . Measurement of fetal forelimb movements in lambs in utero. Am J Obstet Gynecol 1981; 158: 545.
Manning FA, Platt LD, Sipos L . Fetal movements in human pregnancy in the third trimester. Obstet Gynecol 1979; 54: 699.
Cohn HE, Sacks EJ, Heyman MA, Rudolph AM . Cardiovascular responses to hypoxemia and acidemia in fetal lambs. Am J Obstet Gynecol 1974; 120: 817–824.
Manning FA, Platt LD, Sipos L . Antepartum fetal evaluation: development of a fetal biophysical profile. Am J Obstet Gynecol 1980; 136: 787–795.
Lumly J, Lester A, Anderson I, Renou P, Wood C . A randomized trial of weekly cardiotocography in high-risk obstetrical patients. BJOG 1983; 90: 1018–1026.
Kidd LC, Patel N, Smith R . Non-stress cardiotocography—a prospective randomized clinical trial. BJOG 1985; 92: 1156–1159.
Boehm FH . Improved outcome of twice weekly nonstress testing. Obstet Gynecol 1986; 67 (4): 566–568.
Platt LD, Walla CA, Paul RH, Trujillo ME, Loesser CV, Jacobs ND et al. A prospective trial of the fetal biophysical profile versus the nonstress test in the management of high-risk pregnancies. Am J Obstet Gynecol 1985; 153: 624–633.
Manning FA, Snijders RL, Harman CR, Nicolaides K, Menticoglou S, Morrison I . Fetal biophysical profile score. VI: correlation with antepartum umbilical venous pH. Am J Obstet Gynecol 1993; 169: 755–763.
Bocking AD, Gagnon R, Milne KM, White SE . Behavioral activity during prolonged hypoxemia in fetal sheep. J App Physiol 1988; 65: 2420–2426.
Manning FA, Baskett TF, Morrison I, Lange I . Fetal biophysical profile scoring: a prospective study in 1184 high-risk patients. Am J Obstet Gynecol 1981; 140: 525–530.
Manning FA, Morrison I, Lange IR, Harman CR, Chamberlain PF . Fetal assessment based on fetal biophysical profile scoring: experience in 12,620 referred high-risk pregnancies. I. Perinatal mortality by frequency and etiology. Am J Obstet Gynecol 1985; 151: 343–350.
Manning FA, Morrison I, Lange IR, Harman CR, Chamberlain PFC . Fetal biophysical profile: selective use of the nonstress test. Am J Obstet Gynecol 1987; 56: 709–712.
Vintzileos AM, Campbell WA, Ingardia CJ, Nochimson DJ . The fetal biophysical profile and its predictive value. Obstet Gynecol 1983; 62: 271–278.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Denney, J., Waters, T., Gorman, R. et al. Choice of antenatal testing significantly effects a patient's work obligations. J Perinatol 28, 102–106 (2008). https://doi.org/10.1038/sj.jp.7211877
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211877