Abstract
Objective
To determine the effect of different regimen of first hour fluid administration rates on mortality and severe consequences of impaired circulation in 2 to 60 months old children with impaired circulation.
Design
Systematic review of randomized controlled trials.
Data sources
Various databases including PubMed, Cochrane Library and EMBASE were searched.
Results
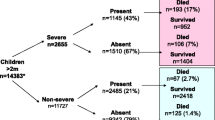
We found only two relevant trials; one was excluded as there was no comparator arm. Only one study (The FEAST Trial) compared boluses with maintenance fluid alone in children with severe febrile illness and one or more signs of impaired perfusion. The 48-hour mortality was more in the bolus group (RR 1.45, 95% CI 1.13,1.86). The quality of evidence is rated as ‘moderate’. For the children who met the WHO criteria for shock (severely impaired circulation) (n=65 children), those receiving boluses had higher mortality (RR 2.40, 95% CI 0.84, 6.88); the quality of evidence was rated as ‘very low’.
Conclusions
A single large randomized controlled trial conducted in low-resource settings indicates that administration of fluid bolus is associated with higher mortality in comparison to the maintenance fluids alone in children with severe febrile illness and one or more signs of impaired perfusion. The findings are not generalizable to contexts with different severity of and different causes of shock and in centers with better facilities. There is urgent need for research in different settings to determine the optimal rate of fluid resuscitation in the first hour in children presenting with impaired circulation, particularly with severely impaired circulation.
Similar content being viewed by others
References
Bhutta ZA, Black RE. Global maternal, newborn, and child health–so near and yet so far. N Engl J Med. 2013;369: 2226–35.
Sarthi M, Lodha R, Vivekanandhan S, Arora NK. Adrenal status in children with septic shock using low-dose stimulation test. Pediatr Crit Care Med. 2007;8:23–8.
Proulx F, Fayon M, Farrell CA, Lacroix J, Gauthier M. Epidemiology of sepsis and multiple organ dysfunction syndrome in children. Chest. 1996;109:1033–7.
Finfer S, Bellomo R, Boyce N, French J, Myburgh J, Norton R, et al. A comparison of albumin and saline for fluid resuscitation in the intensive care unit. N Engl J Med. 2004;350:2247–56.
Brierley J, Carcillo JA, Choong K, Cornell T, Decaen A, Deymann A, et al. Clinical practice parameters for hemodynamic support of pediatric and neonatal septic shock: 2007 update from the American College of Critical Care Medicine. Crit Care Med. 2009;37:666–88.
WHO Pocket Book of Hospital Care for Children: Guidelines for the Management of Common Illnesses with Limited Resources. Available from: http://www.asha.org/ Members/ebp/compendium/guidelines/WHO-Pocket-Book-of-Hospital-Care-for-Children–Guidelines-forthe-Management-of-Common-Illnesses-with-Limited-Resources.htm
Brilli RJ, Goldstein B. Pediatric sepsis definitions: Past, present, and future. Pediatr Crit Care Med. 2005;6:S6–8.
Maitland K, Kiguli S, Opoka RO, Engoru C, Olupot- Olupot P, Akech SO, et al. Mortality after fluid bolus in African children with severe infection. N Engl J Med. 2011;364:2483–95.
Higgins JPT GS. Selecting studies and collecting data. Cochrane Handbook for Systematic reviews of interventions. West Sussex, England: John Wiley & Sons Ltd; 2008. p. 151–86.
Green S HJ. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. The Cochrane Collaboration. 2011.
Schünemann HJ, Oxman AD, Vist GE, Higgins JPT, Deeks JJ, Glasziou P, et al. Chapter 12: Interpreting results and drawing conclusions. In: Higgins JPT, Green S, editors. Cochrane Handbook for Systematic Reviews of Interventions [Internet]. Version 5.1.0. The Cochrane Collaboration, 2011. Available from: www.cochranehandbook. org. Accessed April 01, 2015.
Sterne JAC, Smith GD. Investigating and dealing with publication and other biases. In: Smith GD, editor. Systematic Reviews in Health Care: Meta-analysis in Context. London: BMJ Books; 2001. p. 189–208.
Sterne JAC, Harbord RM. Funnel plots in meta-analysis. Stata J. 2004;4:127–41.
Sterne JAC, Bradburn MJ, Egger M. Meta-analysis in STATA. In: Egger M, Smith GD, Altman DG. Systematic Reviews in Health Care: Meta-analysis in context. London: BMJ Books; 2001. p. 347–69.
Santhanam I, Sangareddi S, Venkataraman S, Kissoon N, Thiruvengadamudayan V. A prospective randomized controlled study of two fluid regimens in the initial management of septic shock in the emergency department. Pediatr Emerg Care. 2008;24:647–55.
Maitland K, George EC, Evans JA, Kiguli S, Olupot- Olupot P, Akech SO, et al. Exploring mechanisms of excess mortality with early fluid resuscitation: insights from the FEAST trial. BMC Med. 2013;11:68.
Kiguli S, Akech SO, Mtove G, Opoka RO, Engoru C, Olupot-Olupot P, et al. WHO guidelines on fluid resuscitation in children: missing the FEAST data. BMJ. 2014;348:f7003.
American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference: Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med. 1992;20:864–74.
Task force of the American College of Critical Care Medicine, Society of Critical Care Medicine. Practice parameters for hemodynamic support of sepsis in adults with sepsis. Crit Care Med. 1999;27:695–7.
Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, Opal SM, et al. Surviving Sepsis Campaign Guidelines Committee including the Pediatric Subgroup. Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock: 2012. Crit Care Med. 2013;41:580–637.
de Oliveira CF, de Oliveira DS, Gottschald AF. ACCM/ PALS haemodynamic support guidelines for paediatric septic shock: An outcomes comparison with and without monitoring central venous oxygen saturation. Intensive Care Med. 2008;34:1065–75.
Ford N, Hargreaves S, Shanks L. Mortality after fluid bolus in children with shock due to sepsis or severe infection: A systematic review and meta-analysis. PLoS One. 2012;7:e43953.
Opiyo N, Molyneux E, Sinclair D, Garner P, English M. Immediate fluid management of children with severe febrile illness and signs of impaired circulation in lowincome settings: A contextualised systematic review. BMJ Open. 2014;4:e004934.
Duke T. What the African fluid-bolus trial means. Lancet. 2011;378:1685–7.
Otiena H, Were E, Agmed I, Brent A, Maitland K. Are bedside features of shock reproducible between different observers? BMJ. 2004;89:979.
Scott H, Melendez E, Cruz AT; American Academy of Pediatrics, Section on Emergency Medicine, Septic Shock Collaborative. Mortality after fluid bolus in African children with sepsis. N Engl J Med. 2011;365:1350–1.
Berend K. Mortality after fluid bolus in African children with sepsis. N Engl J Med. 2011;365:1349.
Ford SR, Visram A. Mortality after fluid bolus in African children with sepsis. N Engl J Med. 2011;365:1348.
Kissoon N, Carcillo JA, Global Sepsis Initiative of the World Federation of Pediatric Intensive and Critical Care Societies. Mortality after fluid bolus in African children with sepsis. N Engl J Med. 2011;365:1350.
Joyner BL Jr, Boyd JM, Kocis KC. Mortality after fluid bolus in African children with sepsis. N Engl J Med. 2011;365:1349–50.
Duke T, Molyneux EM. Intravenous fluids for seriously ill children: time to reconsider. Lancet. 2003;362:1320–3.
Dhawan A, Narang A, Singhi S. Hyponatremia and the inappropriate ADH syndrome in pneumonia. Ann Trop Paediatr. 1992;12:455–62.
Duke T, Mokela D, Frank D. Management of meningitis in children with oral fluid restriction or intravenous fluid at maintenance volumes: a randomised trial. Ann Trop Pediatr. 2002;22:145–57.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tripathi, A., Kabra, S., Sachdev, H. et al. Mortality and other outcomes in relation to first hour fluid resuscitation rate: A systematic review . Indian Pediatr 52, 965–972 (2015). https://doi.org/10.1007/s13312-015-0754-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-015-0754-3