Abstract
Purpose
To evaluate the preventive effects of topical skin disinfection with chlorhexidine on bloodstream infection (BSI) associated with totally implantable venous port (Port-A).
Methods
Two consecutive cohorts of solid cancer patients were prospectively followed for the occurrence of Port-A associated BSI (PABSI). The first cohort used povidone–iodine as topical skin disinfection and the second cohort used chlorhexidine. The primary endpoint was the time to first PABSI. Propensity score analysis was applied. The preventive effects of chlorhexidine were analyzed by Cox proportional hazards models.
Results
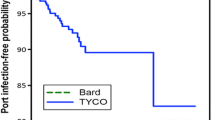
There were 396 patients (81,752 catheter-days) in the iodine cohort and 497 (99,977 catheter-days) in the chlorhexidine cohort. Gram-negative bacteria were the most common pathogens to cause first episode of PABSI (iodine cohort (I) vs chlorhexidine cohort (C) and 0.404 vs 0.450 per 1,000 catheter-day), followed by Gram-positive bacteria (I vs C and 0.269 vs 0.110 per 1,000 catheter-day), and fungi (I vs C and 0.098 vs 0.070 per 1,000 catheter-day). Three hundred forty-three patients were selected from each cohort by propensity score match analysis. Chlorhexidine use was associated with a significant improvement on time to first PABSI caused by Gram-positive bacteria (log-rank test, p = 0.00175; HR = 0.35, 95 % CI, 0.14–0.85, p = 0.02). No significant preventive effects of chlorhexidine on time to first PABSI caused by Gram-negative bacteria or fungi was found.
Conclusions
Chlorhexidine topical skin disinfection may prevent PABSI caused by Gram-positive bacteria in patients with solid cancers. The nonsignificant effect on preventing overall PABSI may be attributed to the high incidence of Gram-negative bacteria related PABSI.



Similar content being viewed by others
References
Biffi R, de Braud F, Orsi F, Pozzi S, Mauri S, Goldhirsch A, Nole F, Andreoni B (1998) Totally implantable central venous access ports for long-term chemotherapy. A prospective study analyzing complications and costs of 333 devices with a minimum follow-up of 180 days. Ann Oncol 9:767–773
Blot SI, Depuydt P, Annemans L, Benoit D, Hoste E, De Waele JJ, Decruyenaere J, Vogelaers D, Colardyn F, Vandewoude KH (2005) Clinical and economic outcomes in critically ill patients with nosocomial catheter-related bloodstream infections. Clin Infect Dis 41:1591–1598
Renaud B, Brun-Buisson C (2001) Outcomes of primary and catheter-related bacteremia. A cohort and case–control study in critically ill patients. Am J Respir Crit Care Med 163:1584–1590
Chen IC, Hsu C, Chen YC, Chien SF, Kao HF, Chang SY, Hu FC, Yeh KH (2013) Predictors of bloodstream infection associated with permanently implantable venous port in solid cancer patients. Ann Oncol 24:463–468
Maki DG, Kluger DM, Crnich CJ (2006) The risk of bloodstream infection in adults with different intravascular devices: a systematic review of 200 published prospective studies. Mayo Clin Proc 81:1159–1171
Mermel LA, Allon M, Bouza E, Craven DE, Flynn P, O’Grady NP, Raad II, Rijnders BJ, Sherertz RJ, Warren DK (2009) Clinical practice guidelines for the diagnosis and management of intravascular catheter-related infection: 2009 Update by the Infectious Diseases Society of America. Clin Infect Dis 49:1–45
Raad I, Hanna H, Maki D (2007) Intravascular catheter-related infections: advances in diagnosis, prevention, and management. Lancet Infect Dis 7:645–657
Bleasdale SC, Trick WE, Gonzalez IM, Lyles RD, Hayden MK, Weinstein RA (2007) Effectiveness of chlorhexidine bathing to reduce catheter-associated bloodstream infections in medical intensive care unit patients. Arch Intern Med 167:2073–2079
O’Grady NP, Alexander M, Burns LA, Dellinger EP, Garland J, Heard SO, Lipsett PA, Masur H, Mermel LA, Pearson ML, Raad II, Randolph AG, Rupp ME, Saint S (2011) Guidelines for the prevention of intravascular catheter-related infections. Clin Infect Dis 52:e162–e193
Vernon MO, Hayden MK, Trick WE, Hayes RA, Blom DW, Weinstein RA (2006) Chlorhexidine gluconate to cleanse patients in a medical intensive care unit: the effectiveness of source control to reduce the bioburden of vancomycin-resistant enterococci. Arch Intern Med 166:306–312
Ramphal R (2004) Changes in the etiology of bacteremia in febrile neutropenic patients and the susceptibilities of the currently isolated pathogens. Clin Infect Dis 39(Suppl 1):S25–S31
Wisplinghoff H, Seifert H, Wenzel RP, Edmond MB (2003) Current trends in the epidemiology of nosocomial bloodstream infections in patients with hematological malignancies and solid neoplasms in hospitals in the United States. Clin Infect Dis 36:1103–1110
Cattaneo C, Quaresmini G, Casari S, Capucci MA, Micheletti M, Borlenghi E, Signorini L, Re A, Carosi G, Rossi G (2008) Recent changes in bacterial epidemiology and the emergence of fluoroquinolone-resistant Escherichia coli among patients with haematological malignancies: results of a prospective study on 823 patients at a single institution. J Antimicrob Chemother 61:721–728
Chen CY, Tsay W, Tang JL, Tien HF, Chen YC, Chang SC, Hsueh PR (2010) Epidemiology of bloodstream infections in patients with haematological malignancies with and without neutropenia. Epidemiol Infect 138:1044–1051
Kang CI, Song JH, Chung DR, Peck KR, Yeom JS, Son JS, Wi YM (2012) Bloodstream infections in adult patients with cancer: clinical features and pathogenic significance of Staphylococcus aureus bacteremia. Support Care Cancer 20:2371–2378
Montassier E, Batard E, Gastinne T, Potel G, de La Cochetiere MF (2013) Recent changes in bacteremia in patients with cancer: a systematic review of epidemiology and antibiotic resistance. Eur J Clin Microbiol Infect Dis 32:841–850
Lim KS, Kam PC (2008) Chlorhexidine—pharmacology and clinical applications. Anaesth Intensive Care 36:502–512
Darouiche RO, Wall MJ Jr, Itani KM, Otterson MF, Webb AL, Carrick MM, Miller HJ, Awad SS, Crosby CT, Mosier MC, Alsharif A, Berger DH (2010) Chlorhexidine-alcohol versus povidone-iodine for surgical-site antisepsis. N Eng J Med 362:18–26
Soofi S, Cousens S, Imdad A, Bhutto N, Ali N, Bhutta ZA (2012) Topical application of chlorhexidine to neonatal umbilical cords for prevention of omphalitis and neonatal mortality in a rural district of Pakistan: a community-based, cluster-randomised trial. Lancet 379:1029–1036
Chaiyakunapruk N, Veenstra DL, Lipsky BA, Saint S (2002) Chlorhexidine compared with povidone-iodine solution for vascular catheter-site care: a meta-analysis. Ann Intern Med 136:792–801
Timsit JF, Schwebel C, Bouadma L, Geffroy A, Garrouste-Orgeas M, Pease S, Herault MC, Haouache H, Calvino-Gunther S, Gestin B, Armand-Lefevre L, Leflon V, Chaplain C, Benali A, Francais A, Adrie C, Zahar JR, Thuong M, Arrault X, Croize J, Lucet JC (2009) Chlorhexidine-impregnated sponges and less frequent dressing changes for prevention of catheter-related infections in critically ill adults: a randomized controlled trial. JAMA 301:1231–1241
Chuang YC, Chen YC, Chang SC, Sun CC, Chang YY, Chen ML, Hsu LY, Wang JT (2010) Secular trends of healthcare-associated infections at a teaching hospital in Taiwan, 1981-2007. J Hosp Infect 76:143–149
Eggimann P (2007) Diagnosis of intravascular catheter infection. Curr Opin Infect Dis 20:353–359
Shen YC, Hsu C, Chen LT, Cheng CC, Hu FC, Cheng AL (2010) Adjuvant interferon therapy after curative therapy for hepatocellular carcinoma (HCC): a meta-regression approach. J Hepatol 52:889–894
D’Agostino RB Jr (1998) Propensity score methods for bias reduction in the comparison of a treatment to a non-randomized control group. Stat Med 17:2265–2281
Snaterse M, Ruger W, Scholte Op Reimer WJ, Lucas C (2010) Antibiotic-based catheter lock solutions for prevention of catheter-related bloodstream infection: a systematic review of randomised controlled trials. J Hosp Infect 75:1–11
van de Wetering MD, van Woensel JB (2007) Prophylactic antibiotics for preventing early central venous catheter Gram positive infections in oncology patients. Cochrane Database Syst Rev 24, CD003295
Yahav D, Rozen-Zvi B, Gafter-Gvili A, Leibovici L, Gafter U, Paul M (2008) Antimicrobial lock solutions for the prevention of infections associated with intravascular catheters in patients undergoing hemodialysis: systematic review and meta-analysis of randomized, controlled trials. Clin Infect Dis 47:83–93
D’Agostino RB Jr, D’Agostino RB Sr (2007) Estimating treatment effects using observational data. JAMA 297:314–316
Novikov I, Kalter-Leibovici O (2007) Analytic approaches to observational studies with treatment selection bias. JAMA 297:2077
Acknowledgments
This study was supported by grants NTUH-100-S1805 from the National Taiwan University Hospital and DOH100-TD-C-111-001 from the Department of Health, Taiwan.
Conflict of interest
None to declare
Author information
Authors and Affiliations
Corresponding author
Additional information
Hsiang-Fong Kao, I-Chun Chen, and Chiun Hsu contributed equally to this work.
Rights and permissions
About this article
Cite this article
Kao, HF., Chen, IC., Hsu, C. et al. Chlorhexidine for the prevention of bloodstream infection associated with totally implantable venous ports in patients with solid cancers. Support Care Cancer 22, 1189–1197 (2014). https://doi.org/10.1007/s00520-013-2071-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-013-2071-5