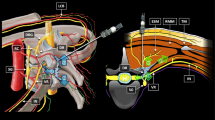
Abstract
The complications of failure, neural injury and local anaesthetic toxicity are common to all regional anaesthesia techniques, and individual techniques are associated with specific complications. All potential candidates for regional anaesthesia should be thoroughly evaluated and informed of potential complications. If there is significant risk of injury, then these techniques should be avoided.
Central neural blockade (CNB) still accounts for more than 70% of regional anaesthesia procedures. Permanent neurological injury is rare (0.02 to 0.07%); however, transient injuries do occur and are more common (0.01 to 0.8%). Pain on injection and paraesthesiae while performing regional anaesthesia are danger signals of potential injury and must not be ignored.
The incidence of systemic toxicity to local anaesthetics has significantly reduced in the past 30 years, from 0.2 to 0.01%. Peripheral nerve blocks are associated with the highest incidence of systemic toxicity (7.5 per 10 000) and the lowest incidence of serious neural injury (1.9 per 10 000).
Intravenous regional anaesthesia is one of the safest and most reliable forms of regional anaesthesia for short procedures on the upper extremity. Brachial plexus anaesthesia is one of the most challenging procedures. Axillary blocks are performed most frequently and are safer than supraclavicular approaches.
Ophthalmic surgery is particularly suited to regional anaesthesia. Serious risks include retrobulbar haemorrhage, brain stem anaesthesia and globe perforation, but are uncommon with skilled practitioners.
Postdural puncture headache remains a common complication of epidural and spinal anaesthesia; however, the incidence has decreased significantly in the past 2 to 3 decades from 37 to approximately 1%, largely because of advances in needle design.
Backache is frequently linked with CNB; however, other causes should also be considered. Duration of surgery, irrespective of the anaesthetic technique, seems to be the most important factor. The syndrome of transient neurological symptoms is a form of backache that is associated with patient position and use of lidocaine (lignocaine).
Disturbances of micturition are a common accompaniment of CNB, especially in elderly males. Hypotension is the most common cardiovascular disturbance associated with CNB. Severe bradycardia and even cardiac arrest have been reported in healthy patients following neuraxial anaesthesia, with a reported incidence of cardiac arrest of 6.4 per 10 000 associated with spinal anaesthesia. Prompt diagnosis, immediate cardiopulmonary resuscitation and aggressive vasopressor therapy with epinephrine (adrenaline) are required.
New complications of regional anaesthesia emerge occasionally, e.g. cauda equina syndrome with chloroprocaine, microspinal catheters and 5% hyperbaric lidocaine, and epidural haematoma formation in association with low molecular weight heparin. Even so, after 100 years of experience, most discerning physicians appreciate the benefits of regional anaesthesia.







Similar content being viewed by others
References
Köller C. The use of cocaine for producing anaesthesia of the eye [translated and reprinted]. Lancet 1884; II: 990–2
Mattison JB. Cocaine poisoning. Med Surg Rep 1891; 60: 645–50
Bier A. Experiments regarding cocainization of the spinal cord [in German]. Zietschr Chir 1899; 51: 361–9
Kennedy F, Effron AS, Perry G. The grave spinal cord paralysis caused by spinal anesthesia. Surg Gynecol Obstet 1950; 91: 385–98
The Wooley and Roe case. Anaesthesia 1954; 9: 249–70
Finucane BT, Finegan BA. The attitude of the general public towards regional anesthesia. Int Monit 1997; 9(3): 74
Cathelin F, Sicard J. Discovery of epidural anesthesia [translated and published in classical file]. Surv Anesthesiol 1979; 23: 271–3
Report on confidential inquiries into maternal deaths in the United Kingdom 1994–96. London: Her Majesty’s Stationary Office, 1998
Snyder SH. Opiate receptors in the brain. N Engl J Med 1977; 296: 266–71
Horlocker T. Peripheral nerve blocks-regional anesthesia for the new millennium. Reg Anesth Pain Med 1998; 23: 237–40
Adriani J. Reactions to local anesthetics. JAMA 1966; 196: 405–8
Brown DT, Beamish D, Wildsmith JAW. Allergic reactions to an amide local anaesthetic. Br J Anaesth 1981; 53: 435–7
Fisher M, Penninton JC. Allergy to local anaesthesia. Br J Anaesth 1982; 54: 893–4
Curley RK, MacFarlane AW, King CM. Contact sensitivity to the amide anesthetics lidocaine, prilocaine and mepivacaine: case report and review of literature. Arch Dermatol 1986; 122: 924–6
Aldrete JA, Johnson DA. Evaluation of intracutaneous testing for investigation of allergy to local anesthetic agents. Anesth Analg 1970; 49: 173–83
Lambert LA, Lambert DH, Strichartz GR. Irreversible conduction block in isolated nerve by high concentrations of local anesthetics. Anesthesiology 1994; 80: 1082–93
Ravindran RS, Bond VK, Tasch MD, et al. Prolonged neural blockade following regional analgesia with 2-chloroprocaine. Anesth Analg 1980; 59: 447–51
Fibuch EE, Oppek SE. Back pain following epidurally administered Nesacaine MPF. Anesth Analg 1989; 69: 113–5
Stevens RA, Urmey WF, Urquhart BL, et al. Back pain after anesthesia with chloroprocaine. Anesthesiology 1993; 78: 492–7
Schneider M, Ettlin T, Kaufmann M, et al. Transient neurologic toxicity after hyperbaric subarachnoid anesthesia with 5% lidocaine. Anesth Analg 1993; 76: 1154–7
Benoit PW, Belt WD. Some effects of local anesthetic agents on skeletal muscle. Exp Neurol 1972; 34: 264–78
Hall-Craggs EC. Rapid degeneration and regeneration of a whole skeletal muscle following treatment with bupivacaine (Marcain). Exp Neurol 1974; 43: 349–58
Benoit PW. Microscarring in skeletal muscles after repeated exposures to lidocaine with epinephrine. J Oral Surg 1978; 36: 530–3
_Kytta J, Heinon G, Rosenberg PH, et al. Effects of repeated bupivacaine administration on sciatic nerve and surrounding tissue in rats. Acta Anaesthesiol Scand 1986; 30: 625–9
Benoit PW. Reversible skeletal muscle damage after administration of local anesthetics with and with out epinephrine. J Oral Surg 1978; 36: 198–201
Hogan Q, Dobson R, Erikson S, et al. Local anesthetic myotoxicity: a case and review. Anesthesiology 1994; 80: 942–7
Massey Dawkins CJ. An analysis of the complications of extradural and caudal block. Anaesthesia 1969; 24: 554–63
Auroy Y, Narchi P, Messiah A, et al. Serious complications related to regional anesthesia. Anesthesiology 1997; 87: 479–86
Brown DL, Ransom DM, Hall JA, et al. Regional anesthesia and local anesthetic-induced systemic toxicity: seizure frequency and accompanying cardiovascular changes. Anesth Analg 1995; 81: 321–8
Covino BG, Vassalo HG. Pharmacokinetic aspects of local anesthetic agents. In: Local anesthetics. Mechanisms of action and clinical use. New York (NY): Grune & Stratton, 1976: 95–121
Löfotröm JB. Physiologic disposition of local anesthetics. Reg Anesth 1982; 7: 33–8
Englesson S, Grevsten S. The influence of acid-base changes on central nervous system toxicity of local anesthetic agents. II. Acta Anaesthesiol Scand 1974; 18: 88–103
Mather LE, Cousins MJ. Local anesthetics and their current clinical use. Drugs 1979; 18: 185–205
Eidelberg E, Lesse H, Gaulta FP. An experimental model of temporal lobe epilepsy. Studies of the convulsant properties of cocaine. In: Glaser GH, editor. EEG and behaviour. New York (NY): Basic Books, 1963
de Jong RH, Heavner JE. Diazepam prevents local anesthetic seizures. Anesthesiology 1971; 34: 523–31
Covino BG. Pharmacology of local anesthetic agents. In: Rogers MC, Tinker JV, Covino B, et al., editors. Principles and practice of anesthesiology. Vol II. St Louis (MO): Mosby-Year Book, 1993
Clarkson CW, Hondeghem LM. Mechanism for bupivacaine depression of cardiac conduction: fast block of sodium channels during the action potential with slow recovery from block during diastole. Anesthesiology 1985; 62: 396–405
Albright GA. Cardiac arrest following regional anesthesia with etiodocaine or bupivacaine. Anesthesiology 1979; 51: 285–7
McCrae AF, Jozwiak H, McClure JH. Comparison of ropivacaine and bupivacaine in extradural analgesia for the relief of pain in labour. Br J Anaesth 1995; 74: 261–5
Hickey R, Hoffman J, Ramamurthy S. A comparison of ropivacaine 0.5% and bupivacaine 0.5% for brachial plexus block. Anesthesiology 1991; 74: 639–42
Brockway MS, Bannister J, McClure JH, et al. Comparison of extradural ropivacaine and bupivacaine. Br J Anaesth 1991; 66: 31–7
Nancarrow C, Rutten AJ, Runciman WG, et al. Myocardial and cerebral drug concentrations and the mechanism of death after fatal intravenous doses of lidocaine, bupivacaine and ropivacaine in sheep. Anesth Analg 1989; 69: 276–83
Scot DB, Lee A, Fagan D, et al. Acute toxicity of ropivacaine compared with that of bupivacaine. Anesth Analg 1989; 69: 563–9
Polley LS, Columb MO, Naughton NN, et al. Relative potencies of ropivacaine and bupivacaine for epidural analgesia in labor. Anesthesiology 1999; 90: 944–8
Lee A, Fagan D, Lamont M, et al. Disposition kinetics of ropivacaine in humans. Anesth Analg 1989; 62: 889–93
Cox CR, Faccenda KA, Gilhooly C, et al. Extradural S (-)- bupivacaine: comparison with racemic RS-bupivacaine. Br J Anaesth 1998; 80: 289-93
Cox CR, Checketts MR, MacKenzie N, et al. Comparison of S-(-)-bupivacaine with racemic (RS)-bupivacaine in supraclavicular brachial plexus block. Br J Anaesth 1998; 80: 594–8
Burke D, Henderson DJ, Simpson AM, et al. Comparison of 0.25% S-(-)-bupivacaine with 0.25% RS-bupivacaine for epidural analgesia in labour. Br J Anaesth 1999; 83: 750–9
Bardsley H, Girstwood R, Watson N, et al. The local anaesthetic activity of levobupivacaine does not differ from racemic bupivacaine (Marcain): first clinical evidence. Expert Opin Invest Drug 1997; 6: 1883–5
Huang YF, Pryor ME, Mather LE, et al. Cardiovascular and central nervous system effects of intravenous levobupivacaine and bupivacaine in sheep. Anesth Analg 1998; 86: 797–804
Bardsley H, Gristwood R, Baker H, et al. A comparison of the cardiovascular effects of levobupivacaine and rac- bupivaca- ine following intravenous administration to healthy volunteers. Br J Clin Pharmacol 1998; 46: 245–9
Mather LE, Huang YF, Veering B, et al. Systemic and regional pharmacokinetics of levobupivacaine enantiomers in sheep. Anesth Analg 1998; 86: 805–11
Faccenda KA, Morrison LMM. The pharmacokinetics of levobupivacaine and racemic bupivacaine following extradural administration. Reg Anesth Pain Med 1998; 23Suppl.: 52
Faccenda KA, Henderson DJ, Morrison LMM. The pharmacokinetics of levobupivacaine and racemic bupivacaine following extradural administration for elective caesarean section. World Congress of Anesthesiologists 2000; P22.3.38
Kasten GW, Martin ST. Successful cardiovascular resuscitation after massive intravenous bupivacaine overdosage in anesthetized dogs. Anesth Analg 1985; 64: 491–7
Lindgren L, Randall T, Suzuki N, et al. The effect of amrinone on recovery from severe bupivacaine intoxication in pigs. Anesthesiology 1992; 77: 309–15
Yuen EC, Layzer RB, Weitz SR, et al. Neurologic complications in lumbar epidural anesthesia and analgesia. Neurology 1995; 45: 1795–801
Masdeu JC, Breuer AC, Schoene WK. Spinal subarachnoid haematomas: clue to a source of bleeding in traumatic lumbar puncture. Neurology 1979; 29: 872–6
Rigler ML, Drasner K, Krejcie TC, et al. Cauda equina syndrome after continuous spinal anesthesia. Anesth Analg 1991; 72: 275–81
Sage DJ. Major neurologic injury following regional anesthesia. In: Finucane BT, editor. Complications of regional anesthesia. New York (NY): Churchill-Livingstone, 1999; 266–8
Cousins MJ, Veering BT. Epidural neural blockade. In: Cousins MJ, Bridenbaugh PO, editors. Neural blockade in clinical anaesthesia and management of pain. 3rd ed. Philadelphia (PA): Lippincott-Raven; 1998: 310
Renck H. Neurological complications of central nerve blocks. Acta Anaesthesiol Scand 1995; 39: 859–68
Moore DC, Mulroy MF, Thompson GE. Peripheral nerve damage and regional anaesthesia. Br J Anaesth 1994; 73: 435–6
Bromage PR, Benumof JL. Paraplegia following intracord injection during attempted epidural analgesia under general anesthesia. Reg Anesth Pain Med 1998; 23: 104–7
Kindler CH, Seeberger MD, Staender SE. Epidural abscess complicating epidural anaesthesia and analgesia. An analysis of the literature. Acta Anaesthesiol Scand 1998; 42: 614–20
Bromage PR. Spinal epidural abscess: pursuit of vigilance. Br J Anaesth 1993; 70: 471–3
Berman RS, Eisele JH. Bacteremia, spinal anesthesia and development of meningitis. Anesthesiology 1978; 48: 376–7
Burke D, Wildsmith JAW. Meningitis after spinal anaesthesia. Br J Anaesth 1997; 78: 635–6
Wang LP, Hauerberg J, Schimdt JF. Incidence ofspinal epidural abscess after epidural analgesia. Anesthesiology 1999; 91: 1928–36
Kindler C, Seeberger M, Schneider M. Extradural abscess complicating lumbar extradural anaesthesia and analgesia in an obstetric patient. Acta Anaesthesiol Scand 1996; 40: 858–61
Baker AS, Ojemann RG, Swantz MN, et al. Spinal epidural abscess. N Engl J Med 1975; 293: 463–8
Eng RHK, Seligman SJ. Lumbar puncture induced meningitis. JAMA 1981; 245: 1456–9
Usubiaga JE. Neurological complications following epidural anesthesia. Int Anesthesiol Clin 1975; 13: 1–153
Kozody R, Palahniuk RJ, Wade JG, et al. The effect of subarachnoid epinephrine and phenylephrine on spinal cord blood flow. Can Anaesth Soc J 1984; 31: 301–8
Tryba M, Wedel DJ. Central neuraxial block and low molecular weight heparin (enoxaparin): lessons learned from different dosage regimes in two continents. Acta Anaesthesiol Scand 1997; 41: 100–3
Baranowski, AP, Pither CE. A comparison of three methods of axillary brachial plexus anaesthesia. Anaesthesia 1990; 45: 362–5
Smith MP, Sprung J, Zura A, et al. A survey of exposure to regional anesthesia techniques in American anesthesia residency training programs. Reg Anesth Pain Med 1999; 24: 11–6
Kopacz DJ, Bridenbaugh LD. Are anesthesia residency programs failing regional anesthesia? The past, present and future. Reg Anesth 1993; 18: 84–7
Rogers A, Walker N, Schug S, et al. Reduction of postoperative mortality and morbidity with epidural or spinal anasthesia: results from overview of randomised trials. BMJ 2000; 321: 1493–7
Kroll DA, Caplan RA, Posner K, et al. Nerve injury associated with anesthesia. Anesthesiology 1990; 73: 202–7
Cheney FW, Domino KB, Caplan RA, et al. Nerve injury associated with anesthesia. Aclosed claims analysis. Anesthesiology 1999; 90: 1062–9
McIntyre JWR. Regional anesthesia safety. In: Finucane BT, editor. Complications of regional anesthesia. NewYork(NY): Churchill Livingstone, 1999: 10
Shevde K, Panagopoulos G. A survey of 800 patients’ knowledge, attitudes and concerns regarding anesthesia. Anesth Analg 1991; 73: 190–8
Fanelli G, Casati A, Garancini P, et al. Nerve stimulator and multiple injection technique for upper and lower limb blockade: failure rate, patient acceptance and neurologic complications. Anesth Analg 1999; 88: 847–52
Bier A. Uben einen neueun weg lokalanasthesie an den gliedmassen zu erzeugen. Arch Klin Chir 1908; 86: 1007–16
Holmes CM. Intravenous regional analgesia: a useful method of producing analgesia of limbs. Lancet 1963; I: 245–7
Wildsmith JAW. Intravenous regional anaesthesia: essential safeguards. Anaesthesia 1982; 37: 959
Cotev S, Robin C. Experimental studies on intravenous regional anaesthesia using radioactive lidocaine. Acta Anaesthesiol Scand 1969; 36Suppl.: 127–30
Kim DD, Shumman C, Sadr B. Intravenous regional anesthesia for outpatient foot and ankle surgery: a prospective study. Orthopedics 1993; 16: 1109–13
Heath ML. Bupivacaine toxicity and Bier blocks. Anesthesiology 1983; 59: 481
Pitkanen MT, Suzuki N, Rosenberg PH. Intravenous regional anesthesia with 0.5% prilocaine or 0.5% chloroprocaine. A double blind comparison in volunteers. Anaesthesia 1992; 47: 618–9
Mabee JR, Bostwick TL, Burke MK. Iatrogenic compartment syndrome from hypertonic saline injection in Bier block. J Emerg Med 1994; 12: 473–6
Quigley JT, Popich GA, Lanz UB. Compartment syndrome of the forearm and hand: a case report. Clin Orthop 1981; 161: 247–51
Luce EA, Mangubat E. Loss of hand and forearm following Bier block: a case report. J Hand Surg 1983; 8: 280–3
Carney AL, Anderson EM. Tourniquet subclavian steal: brain-stem ischemia and cortical blindness — clinical significance and testing. Adv Neurol 1981; 30: 283–90
Brand L, Papper EM. A comparison of supraclavicular and axillary techniques for brachial plexus blocks. Anesthesiology 1961; 22: 226–9
Hickey R, Garland TA, Ramamurthy S. Subclavian perivascular block: influence of location of paresthesiae. Anesth Analg 1989; 68: 767–71
Urmay WF, Talts KH, Sharrock NE. One hundred percent incidence of hemidiaphragmatic paresis associated with inter-scalene brachial plexus anesthesia as diagnosed by ultrasonography. Anesth Analg 1991; 73: 498–503
Selander D, Edshage S, Wolf T. Paresthesiae or no paresthesiae? Acta Anaesthesiol Scand 1979; 23: 27–33
Barutell C, Vidal F, Raich M, et al. Aneurological complication following interscalene brachial plexus block. Anaesthesia 1980; 35: 365–7
Passannante AN. Spinal anesthesia and permanent neurologic deficit after interscalene block. Anesth Analg 1996; 82: 873–4
Bashein G, Robertson HT, Kennedy Jr WF. Persistent phrenic nerve paresis following interscalene brachial plexus block. Anesthesiology 1985; 63: 102–4
Winnie AP. Plexus anesthesia: I. Perivascular techniques of brachial plexus block. Philadelphia (PA): WB Saunders, 1983: 264–6
Restelli L, Pinciroli D, Conoscente F, et al. Insufficient venous drainage following axillary approach to brachial plexus blockade. Br J Anaesth 1984; 56: 1051–3
Ott B, Neuberger L, Frey HP. Obliteration of the axillary artery after axillary block. Anaesthesia 1989; 44: 773–4
Merrill DG, Brodsky JB, Hintz RH. Vascular insufficiency following axillary block of the brachial plexus. Anesth Analg 1981; 60: 162–4
Al-Khafaji JM, Ellias MA. Incidence of Horner syndrome with interscalene brachial plexus block and its importance in the management of head injury. Anesthesiology 1986; 64: 127
Löfström B, Wennberg A, Wide L. Late disturbances in nerve function after block with local anaesthetic agents. Acta Anaesthesiol Scand 1966; 10: 111–22
Selander D, Sjöstrand J. Longitudinal spread of intraneurally injected local anesthetics. An experimental study of the initial neural distribution following intraneural injections. Acta Anaesthesiol Scand 1978; 22: 622–34
Rice ASC, McMahon SB. Peripheral nerve injury caused by injection needles used in regional anaesthesia: influence of bevel configuration, studied in a rat model. Br J Anaesth 1992; 69: 433–8
Selander D, Dhuner KG, Lundborg G. Peripheral nerve injury due to injection needles used for regional anesthesia: an experimental study of acute effects of needle point trauma. Acta Anaesthesiol Scand 1977; 21: 182–8
Kulenkampff D. Die Anästhesia des plexus brachialis. Zentralbl Chir 1911; 38: 1337–40
Anonymous. Anaesthesia for cataract surgery. Eur J Implant Refract Surg 1993; 5: 1–3
Edge KR, Nicoll JMV. Retrobulbar hemorrhage after 12,500 retrobulbar blocks. Anesth Analg 1993; 76: 1019–22
Hamilton RC. Retrobulbar haemorrhage after retrobulbar blocks. Anesth Analg 1994; 78: 608
Hamilton RC, Gimbel HV, Struin L. Regional anaesthesia for 12,000 cataract extraction and intraocular lens implantation procedures. Can J Anaesth 1988; 35: 615–23
Katsev DA, Drews RC, Rose BT. An anatomic study of retrobulbar needle path length. Ophthalmology 1989; 217: 1221–4
Hamilton RC. Brain stem anesthesia as a complication of regional anesthesia for ophthalmic surgery. Can J Ophthalmol 1992; 27: 323–5
Davis DB, Mandel MR. Posterior peribulbar anesthesia: an alternative to retrobulbar anesthesia. J Cataract Refract Surg 1986; 12: 182–4
Berglin L, Stenkula S, Algvere PV. Ocular perforation during retrobulbar and peribulbar injections. Ophthalmic Surg Lasers 1995; 26: 429–34
Rao VA, Kawatra VK. Ocular myotoxic effects of local anesthetics. Can J Ophth 1988; 23: 171–3
Hunter DG, Lam GC, Guyton DL. Inferior oblique muscle injury from local anesthesia for cataract surgery. Ophthalmology 1995; 102: 501–9
Flaatten H, Rodt SA, Vamnes J, et al. Postdural puncture headache: a comparison between 26- and 29-gauge needles in young patients. Anaesthesia 1989; 44: 147–9
Lambert DH, Hurley RJ, Hertwig L, et al. Role of needle gauge and tip configuration in the production of lumbar puncture headache. Reg Anesth 1997; 22: 66–72
Flaatten H, Felthaus J, Larsen R, et al. Postural post-dural puncture headache after spinal and epidural anaesthesia: a randomized, double blind study. Acta Anaesthesiol Scand 1998; 42: 759–64
Tourtellotte WW, Henderson WG, Tucker RP, et al. A randomized double-blind clinical trial comparing 22 versus 26 gauge needle in the production of the postlumbar puncture syndrome in normal individuals. Headache 1972; 12: 73–9
Crawford JS. Lumbar epidural block in labour: a clinical analysis. Br J Anaesth 1972; 44: 66–74
Gormley JB. Treatment of post-spinal headache. Anesthesiology 1960; 21: 565–5
Marandon JY, Souron V, Charlon D, et al. Blood patch treatment of headache occurring after dural puncture at the thoracic level [in French]. Ann Fr Anesth Reanim 1995; 14: 435–7
Colonna-Romano P, Linton P. Cervical dural puncture and lumbar extradural blood patch. Can J Anaesth 1995; 42: 1143–4
Martin R, Jourdain S, Clairoux M, et al. Duration of decubitus position after epidural blood patch — report of an investigation. Can J Anaesth 1994; 41: 23–5
Palmer JH, Wilson DW, Brown CM. Lumbovertebral syndrome after repeat extradural blood patch. Br J Anaesth 1997; 78: 334–6
Perez M, Olmos M, Garrido FJ. Facial nerve paralysis after epidural blood patch. Reg Anesth 1993; 18: 196–8
Tekkök I, Carter DA, Brinker R. Spinal subdural haematoma as a complication of immediate epidural blood patch. Can J Anaesth 1996; 43: 306–9
Vakharia SB, Thomas PS, Rosenbaum AE, et al. Magnetic resonance imaging of cerebrospinal fluid leak and tamponade effect of blood patch in postdural puncture headache. Anesth Analg 1997; 84: 585–90
Vandam LD, Dripps RD. Long term follow up of 10,098 spinal anesthetics. II. Incidence and analysis of minor sensory neurological defects. Surgery 1955; 38: 463–9
Dripps RD, Vandam LD. Hazards of lumbar puncture. JAMA 1951; 147: 1118–21
Levy L, Randall GI, Pandit SK. Does chloroprocaine (Nesacaine MPF) for epidural anesthesia increase the incidence of backache? Anesthesiology 1989; 71: 476
Hetherington R, Stephens RA, White JL, et al. Subjective experiences of anesthesiologists undergoing epidural anesthesia. Reg Anesth 1994; 19: 284–8
Breen TW, Ransil BJ, Groves PA, et al. Factors associated with back pain after childbirth. Anesthesiology 1994; 81: 29–34
Patel M, Fernando R, Gill P, et al. A prospective study of long-term backache after child birth in primagravidae — the effect of ambulatory epidural analgesia during labour. Int J Obstet Anesth 1995; 4; 187
Russell R, Dundas R, Reynolds F. Long term backache after childbirth: prospective search for causative factors. Br Med J 1996; 312; 1384–8
Brown EM, Elman DS. Postoperative backache. Anesth Analg 1961; 40: 683–5
Naveira FA, Copeland S, Anderson M, et al. Transient neurologic toxicity after spinal anesthesia, or is it myofacial pain? Two case reports. Anesthesiology 1998; 88: 268–70
Hampl K, Schneider M. Transient radicular irritation after spinal anesthesia with xylocain. Acta Anaesthesiol Scand 1999; 43: 359–60
Hampl KF, Schneider MC, Pargger H, et al. Asimilar incidence of transient neurologic symptoms after spinal anesthesia with 2% and 5% lidocaine. Anesth Analg 1996; 83: 1051–4
Hampl KF, Schneider MC, Ummenhofer W, et al. Transient neurologic symptoms after spinal anesthesia. Anesth Analg 1995; 81: 1148–53
Tarkkila P, Huhtala J, Tuominen M. Transient radicular irritation after spinal anaesthesia with hyperbaric 5% lidocaine. Br J Anaesth 1995; 74: 328–9
Hampl KF, Scneider MC, Bont A, et al. Transient radicular irritation after single subarachnoid injection of isobaric 2% lignocaine for spinal anaesthesia. Anaesthesia 1996; 51: 178–81
Pollock JE, Liu SS, Neal JM, et al. Dilution of spinal lidocaine does not alter the incidence of transient neurologic symptoms. Anesthesiology 1999; 90: 445–50
Henderson DJ, Faccenda KA, Morrison LMM. Transient radicular irritation with intrathecal plain lignocaine. Acta Anaesthesiol Scand 1998; 42: 376–8
Pollock JE, Neal JM, Stephenson CA, et al. Prospective study of the incidence of transient radicular irritation in patients undergoing spinal anesthesia. Anesthesiology 1996; 84: 1361–7
Sakura S, Sumi M, Sakaguchi Y, et al. The addition of phenylephrine contributes to the development of transient neurologic symptoms after spinal anesthesia with 0.5% tetracaine. Anesthesiology 1997; 87: 771–8
Hiller A, Rosenberg PH. Transient neurological symptoms after spinal anaesthesia with 4% mepivacaine and 0.5% bupivacaine. Br J Anaesth 1997; 79: 301–5
Salmela L, Aromaa U. Transient radicular irritation after spinal anesthesia with hyperbaric solutions of cerebrospinal fluid-diluted lidocaine 50 mg/ml or mepivacaine 40 mg/ml or bupivacaine 5 mg/ml. Acta Anaesthesiol Scand 1998; 42: 765–9
Kalichman MW, Calcutt NA. Local anesthetic-induced conduction block and nerve fibre injury in streptozotocin-diabetic rats. Anesthesiology 1992; 77: 941–7
Tammela T, Kontturi M, Lukkarinen O. Postoperative urinary retention. I. Incidence and predisposing factors. Scan J Urol Nephrol 1986; 20: 197–201
Asantila R, Rosenberg PH, Scheinn B. Comparison of different methods of postoperative analgesia after thoracotomy. Acta Anaesthesiol Scand 1986; 30: 421–5
Breivik H, Högström H, Niemi G, et al. Safe and effective postoperative pain relief: introduction and continuous quality improvement of comprehensive postoperative pain management programmes. In: Breivik H, editor. Baillières clinical anaesthesiology. London: Bailliere Tindall, 1995: 450
Greene NM. The cardiovascular system. In: Physiology of spinal anesthesia. 3rd ed. Baltimore (MD): Williams and Wilkins, 1981: 116
May LG, Bennet A, Lane AL, et al. Effect of high spinal anesthesia on the cardiac output of normal and hypertensive patients. Am J Med 1949; 7: 251–2
Kappagoda CT, Linden RJ, Snow HM. A reflex increase in heart rate from distension of the junction between the superior vena cava and the right atrium. J Physiol 1972; 220: 177–97
Mark AL. The Bezold-Jarisch reflex revisited: clinical implications of inhibitory reflexes originating in the heart. J Am Coll Cardiol 1983; 1: 90–102
Mackey DC, Carpenter RC, Thompson GE, et al. Bradycardia and asystole during spinal anesthesia: a report of three cases without morbidity. Anesthesiology 1989; 70: 866–8
Caplan RA, Ward RJ, Posner K, et al. Unexpected cardiac arrest during spinal anesthesia: a closed claims analysis of predisposing factors. Anesthesiology 1988; 68: 5–11
Rosenberg JM, Wahr JA, Sung CH, et al. Coronary perfusion pressure during cardiopulmonary resuscitation after spinal anesthesia in dogs. Anesth Analg 1996; 82: 84–7
Caplan RA. The ASA closed claims project: lessons learned. ASA annual refresher course lectures 1997: 242
Kennedy Jr WF, Bonica JJ, Akamatsu TJ, et al. Cardiovascular and respiratory effects of subarachnoid block in the presence of acute blood loss. Anesthesiology 1968; 29: 29–35
Cohen LI. Asystole during spinal anesthesia in a patient with sick sinus syndrome. Anesthesiology 1988; 68: 787–8
Greene NM. Preganglionic sympathetic blockade in man: a study of spinal anesthesia. Acta Anaesthesiol Scand 1981; 25: 463–9
Vandam LD, Dripps RD. Long term follow up of patients who received 10,098 spinal anesthetics. Syndrome of decreased intracranial pressure (headache and ocular and auditory difficulties). JAMA 1956; 161: 586–91
Vandam LD, Dripps RD. Exacerbation of pre-existing neurologic disease after spinal anesthesia. N Engl J Med 1956; 255: 843–9
Vandam LD, Dripps RD. Long term follow up of patients who received 10,098 spinal anesthetics. IV. Neurological disease incident to traumatic lumbar puncture. JAMA 1960; 172: 1483–7
Dripps RD, Vandam LD. Long term follow-up of patients who received 10,098 spinal anesthetics. JAMA 1954; 16: 1486–91
Dahlgren N, Törnebrandt K. Neurological complications after anaesthesia: a follow-up of 18,000 spinal and epidural anaesthetics performed over three years. Acta Anaesthesiol Scand 1995; 39: 872–80
Moore DC. Lesions of the spinal cord following regional block procedures. In: Thomas CC, editor. Complications ofregional anesthesia. Springfield (MO): Charles C Thomas, 955: 215–6
Ehni G. Significance of the small lumbar spinal canal: cauda equina syndromes due to spondylosis. Part 4: acute compression artificially-induced during operation. J Neurosurg 1969; 31: 507–12
Skouen JS, Wainapel SF, Willock MM. Paraplegia following epidural anesthesia. Acta Neurol Scand 1985; 72: 437–43
Thromboembolic Risk Factors (THRIFT) Group. Risk of and prophylaxis for venous thromboembolism in hospital patients. Br Med J 1992; 305; 567–74
National Institutes of Health Consensus Conference. Prevention of venous thrombosis and pulmonary embolism. JAMA 1986; 256: 744–s9
Holtas S, Heiling M, Lonntoft M. Spontaneous spinal epidural haematoma: findings at MR imaging and clinical correlation. Radiology 1996; 199: 409–13
Tryba M. Epidural regional anaesthesia and low molecular heparin: pro [in German]. Anaesth Intensivmed Notfallmed Schmerzther 1993; 28: 179–81
Vandermeulen EP, Van Aken H, Vermylen J. Anticoagulants and spinal-epidural anesthesia. Anesth Analg 1994; 79: 1165–77
Heit JA. Low-molecular-weight heparin: biochemistry, pharmacology and concurrent drug precautions. Reg Anesth Pain Med 1998; 23Suppl. 2: 135–9
Horlocker TT, Wedel DJ, Offord KP. Does preoperative antiplatelet therapy increase the risk of hemorrhagic complications associated with regional anesthesia? Anesth Analg 1990; 70: 631–4
Horlocker TT, Wedel DJ, Schroeder DR, et al. Preoperative antiplatelet therapy does not increase the risk of spinal hematoma associated with regional anesthesia. Anesth Analg 1995; 80: 303–9
Urmey WF, Rowlingson J. Do antiplatelet agents contribute to the development of perioperative spinal hematoma? Reg Anesth Pain Med 1998; 23Suppl. 2: 146–51
Neuraxial anesthesia and anticoagulation. Reg Anesth 1998; 23 Suppl.2: 129–93
Liu SS, Mulroy MF. Neuraxial anesthesia and analgesia in the presence of standard heparin. Reg Anesth Pain Med 1998; 23Suppl.2: 157–63
Ruff RL, Dougherty JH. Complications of lumbar puncture followed by anticoagulation. Stroke 1981; 12: 879–81
Davis FM, Laurenson VG, Gillespie WJ, et al. Deep vein thrombosis after total hip replacement. A comparison between spinal and general anaesthesia. J Bone Joint Surg 1989; 71: 181–5
Modig J, Borg T, Karlstrom G, et al. Thromboembolism after total hip replacement: role of epidural and general anesthesia. Anesth Analg 1983; 62: 174–80
Sorenson RM, Pace NL. Anesthetic techniques during surgical repair of femoral neck fractures: a meta-analysis. Anesthesiology 1992; 77: 1095–104
Prins MH, Hirsch J. A comparison of general anesthesia and regional anesthesia as a risk factor for deep venous thrombosis following total hip surgery: a critical review. Thromb Haemost 1990; 64: 479–500
Sharrock NE, Cazan MG, Hargett MJL, et al. Changes in mortality after total hip and knee arthroplasty over a ten year period. Anesth Analg 1995; 80: 242–8
Cook TM. Combined spinal-epidural techniques. Anaesthesia 2000; 55: 42–64
Collis RE, Baxandall ML, Srikantharajah ID, et al. Combined spinal epidural analgia with ability to walk throughout labour. Lancet 1993; 341: 767–8
Lyons G, MacDonald R, Mikl B. Combined epidural/spinal anaesthesia for caesarean section: through the needle or in separate spaces? Anaesthesia 1992; 47: 199–201
Albright GA, Forster RM. The safety and efficacy of combined spinal and epidural analgesia/anaesthesia (6,002 blocks) in a community hospital. Reg Anesth Pain Med 1999; 24: 117–25
Norris MC, Grieco WM, Borokowski M, et al. Complications of labor analgesia: epidural versus combined spinal epidural techniques. Anesth Analg 1994; 79: 529–37
Eldor J, Brodsky V. Danger of metallic particles in the spinalepidural spaces using the needle through needle approach. Acta Anaesthesiol Scand 1991; 35: 461
Eldor J. Metallic particles in the spinal-epidural needle technique. Reg Anesth 1994; 19: 219–20
Brownridge P. Spinal anaesthesia in obstetrics. Br J Anaesth 1991; 67: 663
Eldor J, Guedj P. Aseptic meningitis due to metallic particles in the needle-through-needle technique. Reg Anesth 1995; 20: 360
Carrie LES. Metallic fragments and the combined spinal-extradural technique. Br J Anaesth 1992; 69: 662–3
Herman N, Molin J, Knape KG. No additional metal particle formation using the needle through needle combined epidural/spinal technique. Act Anaesthesiol Scand 1996; 40: 227–31
Hargreaves J. Metal particle generation caused by the combined spinal-extradural technique. Br J Anaesth 1993; 70: 706
Robbins PM, Fernando R, Lim GH. Accidental intrathecal insertion of an extradural catheter during combined spinal-epidural anaesthesia for Caesarean section. Br J Anaesth 1995; 75: 55–7
Ferguson DJM. Dural puncture and epidural catheters. Anaesthesia 1992; 47: 272
Holström B, Rawal N, Axelsson K, et al. Risk of catheter migration during combined spinal epidural block: percutaneous epiduroscopy study. Anesth Analg 1995; 80: 747–53
Harding SA, Collis RE, Morgan BM. Meningitis after combined spinal-extradural anaesthesia in obstetrics. Br J Anaesth 1994; 73: 545–7
Cascio M, Heath G. Meningitis following a combined spinalepidural technique in a labouring parturient. Can J Anaesth 1995; 43: 399–402
Bouhemad B, Dounas M, Mercier FJ, et al. Bacterial meningitis following combined spinal-epidural analgesia in labour. Anaesthesia 1998; 53: 292–5
Schröter J, Djamba DW, Hoffman V, et al. Epidural abscess after combined spinal-epidural. Can J Anaesth 1997; 44: 300–4
Dysart RH, Balakrishnan V. Conservative management of extradural abscess complicating spinal-extradural anaesthesia for caesarean section. Br J Anaesth 1997; 78: 591–3
Hawthorne L, Lyons G. Cardiac arrest complicating spinal anaesthesia for caesarean section. Int J Obstet Anesth 1997; 6: 126–9
Acknowledgements
We wish to acknowledge the steadfast and efficient editing of multiple drafts of the text by Marilyn Blake.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Faccenda, K.A., Finucane, B. Complications of Regional Anaesthesia. Drug-Safety 24, 413–442 (2001). https://doi.org/10.2165/00002018-200124060-00002
Published:
Issue Date:
DOI: https://doi.org/10.2165/00002018-200124060-00002