Abstract
Background
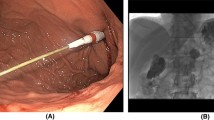
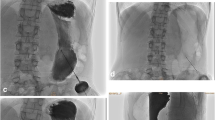
A percutaneous endoscopic gastrostomy (PEG) can be performed as a direct stomach puncture, known as Seldinger technique (“push”) or a thread pulling method (“pull”). The aim of this study was to compare the final results deriving from both application methods.
Methods
Data of all pull-through-PEG and push-PEG applications, which had been carried out in our department from 2009 to 2012, were analyzed and compared retrospectively. Data collection included patients’ demographics, indications, comorbidities, peri-interventional chemotherapy, and/or radiotherapy. The complications were graded according to the Clavien–Dindo classification and divided in early- and late-term complications (before and after 10 days after PEG insertion).
Results
A total of 231 patients received a PEG. Of these, 131 (56.7 %) were treated with pull-through-PEGs and 100 (43.3 %) with the push-PEG method. Overall, in 61 of 231 (26.4 %) patients, a complication was documented and 37 of 61 (60.6 %) were assigned to Clavien–Dindo grade 1. Only 5 of 231 patients (2.2 %) required a re-intervention or surgical treatment under general anesthesia. The overall complication rate was significantly increased by the type of push-PEG tube used (push 33/100 = 33 vs. pull 28/131 = 21.4 %, p = 0.047). A dislocation of the tube was noticed in 5/131 (3.8 %) cases of pull-PEGs and 12/100 (12 %) cases of push PEGs (p = 0.018). An occlusion of the PEG also occurred significantly more frequent in connection with the push-PEG (10/100 = 10 vs. 1/131 = 0.8 %; p < 0.001).
Conclusion
Both PEG techniques are safe and well established. Push PEG showed a significantly higher rate of overall complications, dislocations, and occlusions. The decision which PEG tube should be used depends on individual conditions with preference of push-PEGs in patients with head, neck, and esophageal cancer.
Similar content being viewed by others
References
Gauderer M, Ponsky J, Izant R (1980) Gastrostomy without laparotomy: a percutaneous endoscopic technique. J Pediatr Surg 15:872–875
Kirby D, Delegge M, Fleming C (1995) American Gastroenterological Association technical review on tube feeding for enteral nutrition. Gastroenterology 108:1282–1301
Ponsky J, Gauderer M (1981) Percutaneous endoscopic gastrostomy: a nonoperative technique for feeding gastrostomy. Gastrointest Endosc 27:9–11
Barth C, Stuck B, Hörmann K, Blum A (2007) Postoperative complications in head and neck cancer patients using the pull-through or push-through technique of percutaneous endoscopic gastrostomy. Endo heute 20(2):129–134
Urban K, Terris D (1997) Percutaneous endoscopic gastrostomy by head and neck surgeons. Otolaryngol Head Neck Surg 116:489–492
Akkersdijk W, van Bergeijk J, van Egmond T (1995) Percutaneous endoscopic gastrostomy (PEG): comparison of push and pull methods and evaluation of antibiotic prophylaxis. Endoscopy 27:339–343
Tucker A, Gourin C, Ghegan M (2003) ‘Push’ versus ‘pull’ percutaneous endoscopic gastrostomy tube placement in patients with advanced head and neck cancer. Laryngoscope 113:1898–1902
Kozarek R, Ball T, Ryan J Jr (1986) When push comes to shove: a comparison between two methods of percutaneous endoscopic gastrostomy. Am J Gastroenterol 81:642–646
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Lee C, Im J, Kim J, Kim S, Ryu D, Cha J, Kim E, Chang D (2013) Risk factors for complications and mortality of percutaneous endoscopic gastrostomy: a multicenter, retrospective study. Surg Endosc 27(10):3806–3815
Ermis F, Ozel M, Oncu k, Yazgan Y, Demirtuk L, Gurbuz A, Akyol T, Nazik H (2012) Indications, complications and long-term follow-up of patients undergoing percutaneous endoscopic gastrostomy: a retrospective study. Wien Klin Wochenschr. doi: 10.1007/s00508-011-0082-0
Wilson W, Taubert K, Gewitz M (2007) Prevention of infective endocarditis: guidelines from the American Heart Association: a guideline from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee, Council on Cardiovascular Disease in the Young, and the Council on Clinical Cardiology, Council on Cardiovascular Surgery and Anasthesia, and the Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation 116:1736
Banerjee S, Shen B (2008) Antibiotic prophylaxis for GI endoscopy. Gastrointest Endosc 67:791
Lipp A, Lusardi G (2013) Systemic antimicrobial prophylaxis for percutaneous endoscopic gastrostomy. Cochrane Database Syst Rev. doi:10.1002/14651858.CD005571.pub3
Jafri N, Mahid S, Minor K (2007) Meta-analysis: antibiotic prophylaxis to prevent peristomal infection following percutaneous endoscopic gastrostomy. Aliment Pharmacol Ther 25:647
Adelson R, Ducic Y (2005) Metastatic head and neck carcinoma to a percutaneous endoscopic gastrostomy site. Head Neck 27:339–343
Becker G, Hess C, Grund K, Hoffmann W, Bamberg M (1995) Abdominal wall metastasis following percutaneous endoscopic gastrostomy. Support Care Cancer 3:313–316
Acknowledgments
The authors wish to thank to our Stoma nurses Martina Steinbeiß and Adelheid Anzinger for supplying their records, Babette Dörr for data and quality management, and Norbert Denkmayr and his team of the institute of hygiene for providing supplementary information to our study data. The kind statistical support by Mag. Anita Ferihumer and Univ. Prof. Dr. Helmut Beran is greatly acknowledged.
Disclosures
Gernot Koehler, Veronika Kalcher, Oliver Owen Koch, Ruzica-Rosalia Luketina, Klaus Emmanuel, and Georg Spaun have no conflict of interests or financial ties to disclose. All authors do disclose all institutional or corporate/commercial relationships to all the time of the data collection going back 5 years and longer.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Köhler, G., Kalcher, V., Koch, O.O. et al. Comparison of 231 patients receiving either “pull-through” or “push” percutaneous endoscopic gastrostomy. Surg Endosc 29, 170–175 (2015). https://doi.org/10.1007/s00464-014-3673-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3673-9