Abstract
Purpose
Standardization of care is essential for improving outcome of kidney transplantation (KT). Clinical pathways (CPs) are known to standardize and improve perioperative care for a number of interventions. In transplantation medicine, however, pertinent evidence is very limited. This study evaluates effects of a CP on quality of care in KT.
Materials and methods
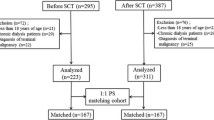
Consecutive patients (n = 32) undergoing KT between July 2006 and August 2007 who were treated with a CP were compared to patients (n = 44) treated without CP between January 2005 and June 2006. Several quality indicators regarding process and outcome were compared between groups.
Results
Quality of care was significantly higher in the CP group for the following indicators: timely removal of central venous catheters, wound drains, and Foley catheters and control of cyclosporine levels, respiratory exercising, and pain control. Median stay decreased non-significantly from 21.4 to 18.3 days. There was significantly less delayed graft function in the CP group. All other outcome indicators showed no significant differences.
Conclusions
Implementation of a CP for KT improves the quality of perioperative treatment by standardizing care. Regarding effects on outcome, no clear conclusion can be drawn. We recommend that large randomized studies are conducted to evaluate the latter issue.

Similar content being viewed by others
References
Abecassis M, Bartlett ST, Collins AJ et al (2008) Kidney transplantation as primary therapy for end-stage renal disease: a National Kidney Foundation/Kidney Disease Outcomes Quality Initiative (NKF/KDOQITM) conference. Clin J Am Soc Nephrol 3(2):471–480
Humar A, Matas AJ (2005) Surgical complications after kidney transplantation. Semin Dial 18(6):505–510
Beyga ZT, Kahan BD (1998) Surgical complications of kidney transplantation. J Nephrol 11(3):137–145
Cecka M (1998) Clinical outcome of renal transplantation. Factors influencing patient and graft survival. Surg Clin North Am 78(1):133–148
Khauli RB (1994) Surgical aspects of renal transplantation: new approaches. Urol Clin North Am 21(2):321–341
Knoll G (2008) Trends in kidney transplantation over the past decade. Drugs 68(Suppl 1):3–10
Schold JD, Srinivas TR, Howard RJ et al (2008) The association of candidate mortality rates with kidney transplant outcomes and center performance evaluations. Transplantation 85(1):1–6
Gjertson DW (2001) Center and other factor effects in recipients of living-donor kidney transplants. Clin Transpl 209–221.
Gjertson DW (1990) Update: center effects. Clin Transpl 375–383
Axelrod DA, Guidinger MK, McCullough KP et al (2004) Association of center volume with outcome after liver and kidney transplantation. Am J Transplant 4(6):920–927
Curtis LT (2008) Prevention of hospital-acquired infections: review of non-pharmacological interventions. J Hosp Infect 69(3):204–219
Humar A, Johnson EM, Gillingham KJ et al (1998) Venous thromboembolic complications after kidney and kidney-pancreas transplantation: a multivariate analysis. Transplantation 65(2):229–234
Kuypers DR (2005) Immunosuppressive drug monitoring—what to use in clinical practice today to improve renal graft outcome. Transpl Int 18(2):140–150
Stiller KR, Munday RM (1992) Chest physiotherapy for the surgical patient. Br J Surg 79(8):745–749
Ronellenfitsch U, Rossner E, Jakob J et al (2008) Clinical Pathways in surgery-should we introduce them into clinical routine? A review article. Langenbecks Arch Surg 393(4):449–457
Holtzman J, Bjerke T, Kane R (1998) The effects of clinical pathways for renal transplant on patient outcomes and length of stay. Med Care 36(6):826–834
Renal transplantation path saves $34 K per patient (1999) Hosp Case Manag 7(1):5–8
Cushing KA, Stratta RJ (1997) Design, development, and implementation of a critical pathway in simultaneous pancreas-kidney transplant recipients. J Transpl Coord 7(4):164–172
Donabedian A (1988) The quality of care. How can it be assessed? JAMA 260(12):1743–1748
Zoccali C, Abramowicz D, Cannata-Andia JB et al (2008) European best practice quo vadis? From European Best Practice Guidelines (EBPG) to European Renal Best Practice (ERBP). Nephrol Dial Transplant 23(7):2162–2166
Ibarra V, Titler MG, Reiter RC (1996) Issues in the development and implementation of clinical pathways. AACN Clin Issues 7(3):436–447
Kinsman L, James E, Ham J (2004) An interdisciplinary, evidence-based process of clinical pathway implementation increases pathway usage. Lippincotts Case Manag 9(4):184–196
Ramos MC, Ratliff C (1997) The development and implementation of an integrated multidisciplinary clinical pathway. J Wound Ostomy Continence Nurs 24(2):66–71
Lied TR, Kazandjian VA (1998) A Hawthorne strategy: implications for performance measurement and improvement. Clin Perform Qual Health Care 6(4):201–204
Zermann DH, Loffler U, Reichelt O et al (2003) Bladder dysfunction and end stage renal disease. Int Urol Nephrol 35(1):93–97
van der Weide MJ, Hilbrands LB, Bemelmans BL et al (2001) Lower urinary tract symptoms after renal transplantation. J Urol 166(4):1237–1241
Delaney CP, Zutshi M, Senagore AJ et al (2003) Prospective, randomized, controlled trial between a pathway of controlled rehabilitation with early ambulation and diet and traditional postoperative care after laparotomy and intestinal resection. Dis Colon Rectum 46(7):851–859
Avital S, Hermon H, Greenberg R et al (2006) Learning curve in laparoscopic colorectal surgery: our first 100 patients. Isr Med Assoc J 8(10):683–686
Acknowledgments
We thank Klaus Meyer, Angela Cepancic, and the whole nursing team for their invaluable help in designing and implementing the CP. We thank the German Society for Process Management (DGKPM) for supporting this project.
Author information
Authors and Affiliations
Corresponding author
Additional information
M. Schwarzbach and R. Bönninghoff contributed equally to the paper.
Rights and permissions
About this article
Cite this article
Schwarzbach, M., Bönninghoff, R., Harrer, K. et al. Effects of a clinical pathway on quality of care in kidney transplantation: a non-randomized clinical trial. Langenbecks Arch Surg 395, 11–17 (2010). https://doi.org/10.1007/s00423-009-0551-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-009-0551-3