Abstract
Background
Numerous epidemiological studies among health care staff have documented associations of adverse psychosocial working conditions with poorer health-related outcomes, a reduced quality of patient care and intentions to leave the profession. The evidence for physician assistants in Germany remains limited though.
Methods
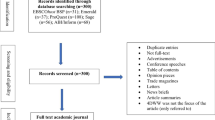
We surveyed a total of 994 physician assistants between September 2016 and April 2017. Psychosocial working conditions were measured by the established effort–reward imbalance (ERI) questionnaire and by a questionnaire specifically developed to capture psychosocial working conditions among physicians. Health outcomes (i.e., self-rated health, depression, anxiety), self-rated quality of care and the intention to leave the profession were assessed by established measures. We ran multivariable logistic regression analyses.
Results
The prevalence of work stress in terms of ERI equalled 73.77%. Work stress according to the ERI model was associated with significantly poorer self-rated health [odds ratio (OR) 3.62], elevated symptoms of depression (OR 8.83) and anxiety (OR 4.95), poorer quality of care (OR for medical errors 4.04; OR for interference of work with patient care 3.88) and an increased intention to leave one’s current profession (OR 3.74). The PA-specific questionnaire showed similar, albeit weaker, associations (all ORs > 1.22).
Conclusions
Our results are in line with previous findings among health care staff and provide specific and novel evidence for physician assistants. Interventions aiming at the improvement of working conditions seem needed given their potential adverse consequences in terms of employee health, quality of care, and personnel policy.
Similar content being viewed by others
References
Angerer P, Weigl M (2015) Physicians’ psychosocial work conditions and quality of care: a literature review. Prof Prof. https://doi.org/10.7577/pp.960
Angerer P, Petru R, Nowak D, Weigl M (2008) Arbeitsbedingungen und Depression bei Ärzten. DMW Dtsch Med Wochenschr 133:26–29. https://doi.org/10.1055/s-2008-1017467
Backé E-M, Seidler A, Latza U et al (2012) The role of psychosocial stress at work for the development of cardiovascular diseases: a systematic review. Int Arch Occup Environ Health 85:67–79. https://doi.org/10.1007/s00420-011-0643-6
Bonde JPE (2008) Psychosocial factors at work and risk of depression: a systematic review of the epidemiological evidence. Occup Environ Med 65:438–445. https://doi.org/10.1136/oem.2007.038430
Degen C, Li J, Angerer P (2015) Physicians’ intention to leave direct patient care: an integrative review. Hum Resour Health. https://doi.org/10.1186/s12960-015-0068-5
Derycke H, Vlerick P, Burnay N et al (2010) Impact of the effort-reward imbalance model on intent to leave among Belgian health care workers: a prospective study. J Occup Organ Psychol 83:879–893. https://doi.org/10.1348/096317909X477594
Dragano N, Siegrist J, Nyberg ST et al (2017) Effort–reward imbalance at work and incident coronary heart disease: a multicohort study of 90,164 individuals. Epidemiology 28:619–626. https://doi.org/10.1097/EDE.0000000000000666
Gavartina A, Zaroti S, Szecsenyi J, Miksch A, Ose D, Campbell SM, Goetz K (2013) Practice assistants in primary care in Germany–associations with organizational attributes on job satisfaction. BMC Fam Pract 14(1):110
Goetz K, Campbell SM, Steinhaeuser J et al (2011) Evaluation of job satisfaction of practice staff and general practitioners: an exploratory study. BMC Fam Pract 12:137
Goetz K, Berger S, Gavartina A et al (2015) How psychosocial factors affect well-being of practice assistants at work in general medical care?—a questionnaire survey. BMC Fam Pract 16. https://doi.org/10.1186/s12875-015-0366-y
Kassenärztliche Bundesvereinigung, GKV-Spitzenverband (2015) Vereinbarung über die Delegation ärztlicher Leistungen an nichtärztliches Personal in der ambulanten vertragsärztlichen Versorgung gemäß § 28 Abs. 1 S. 3 SGB V vom 1, Oktober 2013, Berlin
Kathmann T, Dingeldey I (2013) Prekarisierung berufsfachlich qualifizierter Beschäftigung? Eine Analyse der Arbeitsbedingungen von medizinischen Fachangestellten. Reihe Arbeit und Wirtschaft, Bremen
Kivimaki M, Vahtera J, Elovainio M et al (2007) Effort-reward imbalance, procedural injustice and relational injustice as psychosocial predictors of health: complementary or redundant models? Occup Environ Med 64:659–665. https://doi.org/10.1136/oem.2006.031310
Klein J, Frie KG, Blum K et al (2010) Berufliche Gratifikationskrisen, job strain und Burnout bei chirurgisch tätigen Krankenhausärzten. PPmP Psychother Psychosom Med Psychol 60:374–379. https://doi.org/10.1055/s-0029-1246173
Klein J, Frie KG, Blum K, von dem Knesebeck O (2011) Psychosocial stress at work and perceived quality of care among clinicians in surgery. BMC Health Serv Res. https://doi.org/10.1186/1472-6963-11-109
Kraatz S, Lang J, Kraus T et al (2013) The incremental effect of psychosocial workplace factors on the development of neck and shoulder disorders: a systematic review of longitudinal studies. Int Arch Occup Environ Health 86:375–395. https://doi.org/10.1007/s00420-013-0848-y
Kroenke K, Spitzer RL, Williams JBW, Löwe B (2010) The patient health questionnaire somatic, anxiety, and depressive symptom scales: a systematic review. Gen Hosp Psychiatry 32:345–359. https://doi.org/10.1016/j.genhosppsych.2010.03.006
Kurioka S, Inoue A, Tsutsumi A (2013) Optimum cut-off point of the Japanese short version of the effort-reward imbalance questionnaire. J Occup Health 55:340–348
Lampert T, Kroll LE, von der Lippe E et al (2013) Sozioökonomischer status und Gesundheit: Ergebnisse der Studie zur Gesundheit Erwachsener in Deutschland (DEGS1). Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 56:814–821. https://doi.org/10.1007/s00103-013-1695-4
Larisch M, Joksimovic L, von dem Knesebeck O et al (2003) Berufliche Gratifikationskrisen und depressive Symptome. PPmP Psychother Psychosom Med Psychol 53:223–228
Li J, Galatsch M, Siegrist J et al (2011) Reward frustration at work and intention to leave the nursing profession—prospective results from the European longitudinal NEXT study. Int J Nurs Stud 48:628–635. https://doi.org/10.1016/j.ijnurstu.2010.09.011
Li J, Shang L, Galatsch M et al (2013a) Psychosocial work environment and intention to leave the nursing profession: a cross-national prospective study of eight countries. Int J Health Serv 43:519–536. https://doi.org/10.2190/HS.43.3.i
Li J, Weigl M, Glaser J et al (2013b) Changes in psychosocial work environment and depressive symptoms: a prospective study in junior physicians: changes in ERI and depressive symptoms. Am J Ind Med 56:1414–1422. https://doi.org/10.1002/ajim.22246
Loerbroks A, Meng H, Chen M-L et al (2014) Primary school teachers in China: associations of organizational justice and effort–reward imbalance with burnout and intentions to leave the profession in a cross-sectional sample. Int Arch Occup Environ Health 87:695–703. https://doi.org/10.1007/s00420-013-0912-7
Loerbroks A, Weigl M, Li J, Angerer P (2016) Effort–reward imbalance and perceived quality of patient care: a cross-sectional study among physicians in Germany. BMC Public Health. https://doi.org/10.1186/s12889-016-3016-y
Mark G, Smith AP (2012) Occupational stress, job characteristics, coping, and the mental health of nurses: stress and nurses. Br J Health Psychol 17:505–521. https://doi.org/10.1111/j.2044-8287.2011.02051.x
Msaouel P, Keramaris NC, Apostolopoulos AP et al (2012) The effort–reward imbalance questionnaire in Greek: translation, validation and psychometric properties in health professionals. J Occup Health 54:119–130. https://doi.org/10.1539/joh.11-0197-OA
Nieuwenhuijsen K, Bruinvels D, Frings-Dresen M (2010) Psychosocial work environment and stress-related disorders, a systematic review. Occup Med 60:277–286. https://doi.org/10.1093/occmed/kqq081
Podsakoff PM, MacKenzie SB, Lee J-Y, Podsakoff NP (2003) Common method biases in behavioral research: a critical review of the literature and recommended remedies. J Appl Psychol 88:879–903. https://doi.org/10.1037/0021-9010.88.5.879
Rau R, Henkel D (2013) Zusammenhang von Arbeitsbelastungen und psychischen Erkrankungen: review der Datenlage. Nervenarzt 84:791–798. https://doi.org/10.1007/s00115-013-3743-6
Rössler W (2012) Stress, burnout, and job dissatisfaction in mental health workers. Eur Arch Psychiatry Clin Neurosci 262:65–69. https://doi.org/10.1007/s00406-012-0353-4
Rugulies R, Aust B, Madsen IE (2017) Effort–reward imbalance at work and risk of depressive disorders. A systematic review and meta-analysis of prospective cohort studies. Scand J Work Environ Health 43:294–306. https://doi.org/10.5271/sjweh.3632
Siegrist J (2012) Die ärztliche Rolle im Wandel. Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz 55:1100–1105. https://doi.org/10.1007/s00103-012-1527-y
Siegrist J, Starke D, Chandola T et al (2004) The measurement of effort–reward imbalance at work: European comparisons. Soc Sci Med 58:1483–1499. https://doi.org/10.1016/S0277-9536(03)00351-4
Statistisches Bundesamt (Destatis) (2016a) Staat & Gesellschaft - Berufliche Bildung - Neu abgeschlossene Ausbildungsverträge. Wiesbaden
Statistisches Bundesamt (Destatis) (2016b) Staat & Gesellschaft - Berufliche Bildung - Weibliche Auszubildende. Wiesbaden
Statistisches Bundesamt (Destatis) (2017) Anzahl der Beschäftigten im Gesundheitswesen 2015 in Deutschland nach Berufen, Einrichtungen, Art der Beschäftigung. Alter und Geschlecht, Wiesbaden
Szecsenyi J, Goetz K, Campbell S et al (2011) Is the job satisfaction of primary care team members associated with patient satisfaction? BMJ Qual Saf 20:508–514. https://doi.org/10.1136/bmjqs.2009.038166
Trybou J, Germonpre S, Janssens H et al (2014) Job-related stress and sickness absence among Belgian nurses: a prospective study: job-related stress among nurses. J Nurs Scholarsh 46:292–301. https://doi.org/10.1111/jnu.12075
Tsutsumi A, Kawanami S, Horie S (2012) Effort–reward imbalance and depression among private practice physicians. Int Arch Occup Environ Health 85:153–161. https://doi.org/10.1007/s00420-011-0656-1
Viehmann A, Kersting C, Thielmann A, Weltermann B (2017) Prevalence of chronic stress in general practitioners and practice assistants: personal, practice and regional characteristics. PLOS ONE 12:e0176658. https://doi.org/10.1371/journal.pone.0176658
Virtanen P, Oksanen T, Kivimaki M et al (2008) Work stress and health in primary health care physicians and hospital physicians. Occup Environ Med 65:364–366. https://doi.org/10.1136/oem.2007.034793
von dem Knesebeck O, Klein J, Grosse Frie K et al (2010) Psychosocial stress among hospital doctors in surgical fields: results of a Nationwide Survey in Germany. Dtsch Aerzteblatt Online. https://doi.org/10.3238/arztebl.2010.0248
Vu-Eickmann P, Loerbroks A (2017a) Psychosoziale Arbeitsbedingungen Medizinischer Fachangestellter: Ergebnisse einer qualitativen Studie zu den berufsspezifischen Belastungen, Ressourcen, Präventionsmöglichkeiten und Interventionsbedürfnissen. Zeitschrift für Evidenz, Fortbildung und Qualität im Gesundheitswesen 126:43–51. https://doi.org/10.1016/j.zefq.2017.06.005
Vu-Eickmann P, Loerbroks A (2017b) Psychosoziale Arbeitsbedingungen und Versorgungsqualität: Ergebnisse einer qualitativen Studie unter Medizinischen Fachangestellten (MFAs). Gesundheitswesen 79:1–4 (in press)
Weigl M, Hornung S, Angerer P et al (2013) The effects of improving hospital physicians working conditions on patient care: a prospective, controlled intervention study. BMC Health Serv Res 13:1
West CP, Huschka MM, Novotny PJ et al (2006) Association of perceived medical errors with resident distress and empathy: a prospective longitudinal study. JAMA 296:1071. https://doi.org/10.1001/jama.296.9.1071
Acknowledgements
This study was funded by the Research Commission of the Medical Faculty of the University of Düsseldorf. We are grateful to the PAs for their participation in our study. We would also like to thank in particular the Association of Medical Professionals (VMF e.V.) for supporting our recruitment efforts as main cooperation partner. In addition, we are indebted to Dr. Mergenthal from the Institute for General Practice in Frankfurt for her recruitment support (via “AG WiForMFA” at the 2016 DEGAM Congress). We would also like to thank the following persons and institutions: (a) for forwarding study information to PAs in registered physician practices: association of statutory health insurance physicians Saarland and Mrs. Insa Seeger from the Department of Healthcare Research at the Carl von Ossietzky University of Oldenburg, (b) for forwarding study information to vocational training PA schools: association of statutory health insurance physicians Hamburg, (c) for distribution via internal distribution list and/or publication on their homepage: association of statutory health insurance physicians Brandenburg; section press and media of the association of statutory health insurance physicians Nordrhein; association of statutory health insurance physicians Sachsen; medical association Hamburg; Mr. Paul Hauschild, Managing Director of the local medical association of Trier; and Dr. Müller-Sacks of BAD GmbH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Vu-Eickmann, P., Li, J., Müller, A. et al. Associations of psychosocial working conditions with health outcomes, quality of care and intentions to leave the profession: results from a cross-sectional study among physician assistants in Germany. Int Arch Occup Environ Health 91, 643–654 (2018). https://doi.org/10.1007/s00420-018-1309-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00420-018-1309-4