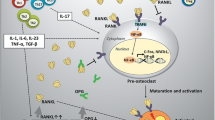
Abstract
Summary
Recently, the use of the pharmacological agent strontium ranelate has come to prominence for the treatment of osteoporosis. While much investigation is focused on preventing disease progression, here we fabricate strontium-containing scaffolds and show that they enhance bone defect healing in the femurs of rats induced by ovariectomy.
Introduction
Recently, the use of the pharmacological agent strontium ranelate has come to prominence for the treatment of osteoporosis due to its ability to prevent bone loss in osteoporotic patients. Although much emphasis has been placed on using pharmacological agents for the prevention of disease, much less attention has been placed on the construction of biomaterials following osteoporotic-related fracture. The aim of the present study was to incorporate bioactive strontium (Sr) trace element into mesoporous bioactive glass (MBG) scaffolds and to investigate their in vivo efficacy for bone defect healing in the femurs of rats induced by ovariectomy.
Methods
In total, 30 animals were divided into five groups as follows: (1) empty defect (control), (2) empty defects with estrogen replacement therapy, (3) defects filled with MBG scaffolds alone, (4) defects filled with MBG + estrogen replacement therapy, and (5) defects filled with strontium-incorporated mesopore-bioglass (Sr-MBG) scaffolds.
Results
The two groups demonstrating the highest levels of new bone formation were the defects treated with MBG + estrogen replacement therapy and the defects receiving Sr-MBG scaffolds as assessed by μ-CT and histological analysis. Furthermore, Sr scaffolds had a reduced number of tartrate-resistant acid phosphatase-positive cells when compared to other modalities.
Conclusion
The results from the present study demonstrate that the local release of Sr from bone scaffolds may improve fracture repair. Future large animal models are necessary to investigate the future relationship of Sr incorporation into biomaterials.






Similar content being viewed by others
References
Fini M, Giavaresi G, Torricelli P, Borsari V, Giardino R, Nicolini A, Carpi A (2004) Osteoporosis and biomaterial osteointegration. Biomed Pharmacother 58:487–493
Fini M, Carpi A, Borsari V, Tschon M, Nicolini A, Sartori M, Mechanick J, Giardino R (2010) Bone remodeling, humoral networks and smart biomaterial technology for osteoporosis. Front Biosci (Schol Ed) 2:468–482
Kanis JA, Oden A, McCloskey EV, Johansson H, Wahl DA, Cooper C, Epidemiology IOFWGo, Quality of L (2012) A systematic review of hip fracture incidence and probability of fracture worldwide. Osteoporos Int 23:2239–2256
Catala-Lopez F, Sanfelix-Gimeno G, Tobias A, Hurtado I, Sanfelix-Genoves J, Peiro S (2013) Efficacy of osteoporosis therapies in a network meta-analysis with indirect comparisons: many concerns for new tools of evidence synthesis? Osteoporos Int 24:1927–1928
Zallone A (2006) Direct and indirect estrogen actions on osteoblasts and osteoclasts. Ann N Y Acad Sci 1068:173–179
Almeida M, Iyer S, Martin-Millan M et al (2013) Estrogen receptor-alpha signaling in osteoblast progenitors stimulates cortical bone accrual. J Clin Invest 123:394–404
Richette P, Roux C (2012) Impact of treatments for osteoporosis on cartilage biomarkers in humans. Osteoporos Int 23(Suppl 8):S877–S880
Roux C, Richette P (2012) Impact of treatments for osteoporosis on osteoarthritis progression. Osteoporos Int 23(Suppl 8):S881–S883
Maimoun L, Brennan TC, Badoud I, Dubois-Ferriere V, Rizzoli R, Ammann P (2010) Strontium ranelate improves implant osseointegration. Bone 46:1436–1441
Alegre DN, Ribeiro C, Sousa C, Correia J, Silva L, de Almeida L (2012) Possible benefits of strontium ranelate in complicated long bone fractures. Rheumatol Int 32:439–443
Hiligsmann M, Ben Sedrine W, Bruyere O, Reginster JY (2013) Cost-effectiveness of strontium ranelate in the treatment of male osteoporosis. Osteoporos Int 24:2291–2300
Doublier A, Farlay D, Jaurand X, Vera R, Boivin G (2013) Effects of strontium on the quality of bone apatite crystals: a paired biopsy study in postmenopausal osteoporotic women. Osteoporos Int 24:1079–1087
Li Y, Feng G, Gao Y, Luo E, Liu X, Hu J (2010) Strontium ranelate treatment enhances hydroxyapatite-coated titanium screws fixation in osteoporotic rats. J Orthop Res 28:578–582
Ammann P, Badoud I, Barraud S, Dayer R, Rizzoli R (2007) Strontium ranelate treatment improves trabecular and cortical intrinsic bone tissue quality, a determinant of bone strength. J Bone Miner Res Off J Am Soc Bone Min Res 22:1419–1425
Marie PJ (2006) Strontium ranelate: a dual mode of action rebalancing bone turnover in favour of bone formation. Curr Opin Rheumatol 18(Suppl 1):S11–S15
Kendler DL (2006) Strontium ranelate—data on vertebral and nonvertebral fracture efficacy and safety: mechanism of action. Curr Osteoporos Rep 4:34–39
Yan X, Huang X, Yu C, Deng H, Wang Y, Zhang Z, Qiao S, Lu G, Zhao D (2006) The in-vitro bioactivity of mesoporous bioactive glasses. Biomaterials 27:3396–3403
Wu C, Fan W, Gelinsky M, Xiao Y, Simon P, Schulze R, Doert T, Luo Y, Cuniberti G (2011) Bioactive SrO-SiO2 glass with well-ordered mesopores: characterization, physiochemistry and biological properties. Acta Biomater 7:1797–1806
Saravanapavan P, Hench LL (2001) Low-temperature synthesis, structure, and bioactivity of gel-derived glasses in the binary CaO-SiO2 system. J Biomed Mater Res 54:608–618
Wu C, Chang J, Xiao Y (2011) Mesoporous bioactive glasses as drug delivery and bone tissue regeneration platforms. Ther Deliv 2:1189–1198
Zhang Y, Cheng N, Miron R, Shi B, Cheng X (2012) Delivery of PDGF-B and BMP-7 by mesoporous bioglass/silk fibrin scaffolds for the repair of osteoporotic defects. Biomaterials 33:6698–6708
Wu C, Zhou Y, Lin C, Chang J, Xiao Y (2012) Strontium-containing mesoporous bioactive glass scaffolds with improved osteogenic/cementogenic differentiation of periodontal ligament cells for periodontal tissue engineering. Acta Biomater 8:3805–3815
Zhang Y, Wei L, Chang J, Miron RJ, Shi B, Yi S, Wu C (2013) Strontium-incorporated mesoporous bioactive glass scaffolds stimulating in vitro proliferation and differentiation of bone marrow stromal cells and in vivo regeneration of osteoporotic bone defects. J Mater Chem B 1:5711–5722
Cheng N, Dai J, Cheng X, Li S, Miron RJ, Wu T, Chen W, Zhang Y, Shi B (2013) Porous CaP/silk composite scaffolds to repair femur defects in an osteoporotic model. J Mater Sci Mater Med 24:1963–1975
Miron RJ, Wei L, Bosshardt DD, Buser D, Sculean A, Zhang Y (2013) Effects of enamel matrix proteins in combination with a bovine-derived natural bone mineral for the repair of bone defects. Clin Oral Investig
Wei L, Miron RJ, Shi B, Zhang Y (2013) Osteoinductive and osteopromotive variability among different demineralized bone allografts. Clin Implant Dent Relat Res. doi:10.1111/cid.12118
Alt V, Thormann U, Ray S et al (2013) A new metaphyseal bone defect model in osteoporotic rats to study biomaterials for the enhancement of bone healing in osteoporotic fractures. Acta Biomater 9:7035–7042
Canettieri AC, Colombo CE, Chin CM, Faig-Leite H (2009) Femur bone repair in ovariectomized rats under the local action of alendronate, hydroxyapatite and the association of alendronate and hydroxyapatite. Int J Exp Pathol 90:520–526
Miron RJ, Zhang YF (2012) Osteoinduction: a review of old concepts with new standards. J Dent Res 91:736–744
Barrere F, van Blitterswijk CA, de Groot K (2006) Bone regeneration: molecular and cellular interactions with calcium phosphate ceramics. Int J Nanomedicine 1:317–332
Yu J, Li K, Zheng X, He D, Ye X, Wang M (2013) In vitro and in vivo evaluation of zinc-modified ca-si-based ceramic coating for bone implants. PLoS One 8:e57564
Schilling AF, Linhart W, Filke S, Gebauer M, Schinke T, Rueger JM, Amling M (2004) Resorbability of bone substitute biomaterials by human osteoclasts. Biomaterials 25:3963–3972
Haynes DR, Crotti TN, Zreiqat H (2004) Regulation of osteoclast activity in peri-implant tissues. Biomaterials 25:4877–4885
Acknowledgements
This project was supported by the Program for New Century Excellent Talents in University (NCET-11-0414), Excellent Youth Foundation of Hubei and the funds of the National Natural Science Foundation of China (81271108).
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Lingfei Wei and Jin Ke contributed equally to this work.
Rights and permissions
About this article
Cite this article
Wei, L., Ke, J., Prasadam, I. et al. A comparative study of Sr-incorporated mesoporous bioactive glass scaffolds for regeneration of osteopenic bone defects. Osteoporos Int 25, 2089–2096 (2014). https://doi.org/10.1007/s00198-014-2735-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-014-2735-0