Abstract
Background
Massive hemorrhage is a common cause of death in patients sustaining instable pelvic ring fractures. Pelvic binders have been propagated for rapid, non-invasive pelvic ring stabilization and control of severe pelvic hemorrhage. There is a recommendation to applicate a pelvic binder due to the trauma mechanism alone. However, there is little evidence to support this advice. The aim of this study was to evaluate effects of an early pelvic binder application on transfusion requirements and hospital mortality.
Methods
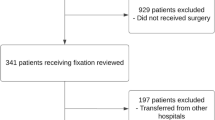
This was a subgroup analysis of a study investigating clinical examination for pelvic stability. We included 64 patients who showed radiologically proven pelvic ring fracture (Tile type B or C). Study data were complemented by retrospective chart review to assess transfusion requirements. We used descriptive statistical analysis.
Results
37 patients had a pelvic binder applied during prehospital treatment (pb), 27 received no binder (npb). Both showed no statistically significant difference in terms of injury severity or probability of survival. We found a trend towards higher ISS (29.7 vs. 24.4) and a lower probability of survival (RISC-II Prognosis 81% vs. 89%) in the pb group. Risk for massive transfusion according to TASH-Scores (10% vs. 6%), and average number of RPBC transfused (10.5 vs. 7.5) was higher in the pb group, without statistically significance. 20 patients (54%) in the pb group and 15 patients (55%) in the npb group showed a need of RPBC within the first 72 h. There was no significant difference in hospital mortality (20% vs. 13.3%).
Conclusion
We were unable to identify blood-saving effects with application of a pelvic binder to patients with instable pelvic ring fractures in terms of RPBC requirements. Nevertheless, some salutary effect of prehospital pb application may be assumed. Better studies are needed to elucidate the value of this intervention.
Similar content being viewed by others
References
Manson T, et al. Young-Burgess classification of pelvic ring fractures: does it predict mortality, transfusion requirements, and non-orthopaedic injuries? J Orthop Trauma. 2010;24(10):603–9.
Mucha P, Welch TJ. Hemorrhage in major pelvic fractures. Surg Clin N Am. 1988;68(4):757–73.
Ward LD, et al. The immediate treatment of pelvic ring disruption with the pelvic stabilizer. Bull Hosp Jt Dis. 1997;56(2):104–6.
Starr AJ, et al. Pelvic ring disruptions: prediction of associated injuries, transfusion requirement, pelvic arteriography, complications, and mortality. J Orthop Trauma. 2002;16(8):553–61.
Lefering R, Paffrath T. Annual_Report_TraumaRegister_DGU_2015. 2016.
Spanjersberg WR, et al. Effectiveness and complications of pelvic circumferential compression devices in patients with unstable pelvic fractures: a systematic review of literature. Injury. 2009;40(10):1031–5.
Tan ECTH, van Stigt SFL, van Vugt AB. Effect of a new pelvic stabilizer (T-POD®) on reduction of pelvic volume and haemodynamic stability in unstable pelvic fractures. Injury. 2010;41(12):1239–43.
Esmer E, Derst P, Schulz M. Influence of external pelvic stabilization on hemodynamically unstable pelvic fractures. Unfallchirurg. 2017;120(4):312–9.
Miller PR, et al. External fixation or arteriogram in bleeding pelvic fracture: initial therapy guided by markers of arterial hemorrhage. J Trauma. 2003;54(3):437–43.
Metz CM, et al. Pelvic fracture patterns and their corresponding angiographic sources of hemorrhage. Orthop Clin N Am. 2004;35(4):431–7.
Pehle B, et al. Significance of physical examination and radiography of the pelvis during treatment in the shock emergency room. Unfallchirurg. 2003;106(8):642–8.
Shlamovitz GZ, et al. How (un)useful is the pelvic ring stability examination in diagnosing mechanically unstable pelvic fractures in blunt trauma patients? J Trauma. 2009;66(3):815–20.
Schweigkofler U, Wohlrath B, Trentsch H, et al. Diagnostics and early treatment in prehospital and emergency-room phase in suspicious pelvic ring fractures. Eur J Trauma Emerg Surg. 2018;44(5):747–752. https://doi.org/10.1007/s00068-017-0860-0.
Evers BM, Cryer HM, Miller FB. Pelvic fracture haemorrhage. Priorities in management. Arch Surg. 1989;124(4):422–4.
Blackmore CC, et al. Predicting major hemorrhage in patients with pelvic fracture. J Trauma. 2006;61(2):346–52.
Gabbe BJ, et al. Predictors of mortality following severe pelvic ring fracture: results of a population-based study. Injury. 2011;42(10):985–91.
Cryer HM, et al. Pelvic fracture classification: correlation with hemorrhage. J Trauma. 1988;28(7):973–80.
Cullinane DC, et al. Eastern Association for the Surgery of Trauma practice management guidelines for hemorrhage in pelvic fracture–update and systematic review. J Trauma. 2011;71(6):1850–68.
Agri F, et al. Association of pelvic fracture patterns, pelvic binder use and arterial angio-embolization with transfusion requirements and mortality rates; a 7-year retrospective cohort study. BMC Surg. 2017;17(1):104.
Ghaemmaghami V, et al. Effects of early use of external pelvic compression on transfusion requirements and mortality in pelvic fractures. Am J Surg. 2007;194(6):720–3.
Esmer E, et al. Influence of external pelvic stabilization on hemodynamically unstable pelvic fractures. Unfallchirurg. 2017;120(4):312–9.
Croce MA, Magnotti LJ, et al. Emergent pelvic fixation in patients with exsanguinating pelvic fractures. J Am Coll Surg. 2007;204(5):935.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
All procedures performed in studies were in accordance with the ethical standards of the national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Schweigkofler, U., Wohlrath, B., Trentzsch, H. et al. Is there any benefit in the pre-hospital application of pelvic binders in patients with suspected pelvic injuries?. Eur J Trauma Emerg Surg 47, 493–498 (2021). https://doi.org/10.1007/s00068-019-01239-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-019-01239-6